Published: 27 February 2026. The English Chronicle Desk. The English Chronicle Online.
An Australian family is mourning an unimaginable loss after a tick bite triggered a fatal meat allergy in their teenage son. The heartbreaking case has drawn international attention, as medical experts confirm it is the first documented death of its kind in Australia. The rare reaction, linked to a condition known as alpha-gal syndrome, has raised urgent questions about awareness and diagnosis.
On a cold evening in June 2022, 16-year-old Jeremy Webb was camping with friends on the New South Wales Central Coast. After eating beef sausages around the campfire, he suddenly became unwell and vomited. Within minutes, he was struggling to breathe and feeling faint. Realising something was terribly wrong, he ran towards a nearby camper van and asked for help. He collapsed soon after knocking on the window, leaving his friends in shock and panic.
His friends immediately began cardiopulmonary resuscitation while waiting for paramedics to arrive. An ambulance reached the remote campsite at 11.26pm and rushed him to hospital. Despite desperate efforts from medical staff, Jeremy was declared dead just over an hour later. His sudden death devastated his family and stunned the local community.
Initially, the tragedy was attributed to a severe asthma attack. Jeremy had lived with asthma for much of his life. However, lingering questions led his parents to push for a detailed coronial inquest. They believed something more complex may have contributed to their son’s final moments.
This week, Deputy NSW State Coroner Carmel Forbes delivered her findings. She concluded Jeremy died from anaphylaxis caused by a mammalian meat allergy following tick bites. The allergic reaction triggered an acute exacerbation of asthma, which ultimately proved fatal. The coroner described the event as a tragic convergence of known risk factors.
According to Professor Sheryl van Nunen of the National Allergy Centre of Excellence, Jeremy appears to be the first documented fatal case of mammalian meat allergy in Australia. She also believes he may have been the first recorded worldwide. A similar case involving a pilot in New Jersey was reported in 2024, but Jeremy’s case predates it.
Professor van Nunen first identified the link between tick bites and meat allergy more than a decade ago. Her pioneering research demonstrated that certain tick species can trigger an immune response to a sugar molecule known as alpha-gal. This molecule is present in many mammals, including cows, sheep, pigs, and kangaroos.
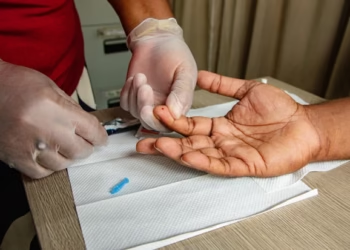
When a tick bites a human, it can transfer alpha-gal through its saliva. In some individuals, repeated bites prompt the immune system to produce antibodies against the molecule. Once sensitised, the person may develop a meat allergy after consuming red meat. Reactions typically occur three to six hours after eating, making diagnosis particularly challenging.
Unlike many food allergies, symptoms are often delayed rather than immediate. Patients may experience abdominal pain, nausea, or hives during the night after a meal. In severe cases, the reaction escalates into life-threatening anaphylaxis. For individuals with asthma, the risk of a fatal outcome increases significantly.
Jeremy had experienced multiple tick bites after his family moved to bushland on the Central Coast. Surrounded by dense vegetation, the area is known for tick activity. Over time, he began reacting to red meat, particularly beef and lamb. His family suspected a connection between the bites and his symptoms.
Despite their concerns, neither Jeremy nor his general practitioner fully understood the potential severity of the condition. Previous hospital visits for breathing difficulties were recorded as asthma episodes. The discharge summaries did not mention anaphylaxis as a possible cause. Professor van Nunen later described this as a missed opportunity for deeper investigation.
The coroner’s report highlighted unusual features in Jeremy’s earlier episodes. His symptoms had an abrupt onset and required repeated doses of adrenaline. He responded positively to the medication, which is consistent with anaphylaxis treatment. Yet the broader pattern linking tick bites and meat allergy remained unrecognised.
Medical experts stress that asthma is a significant risk factor in fatal food allergy cases. Research indicates that up to 85 percent of food allergy deaths involve asthma complications. When an allergic reaction constricts the airways, those with underlying respiratory conditions face amplified danger.
Alpha-gal is found in beef, lamb, pork, goat, venison, and other mammalian meats. It can also appear in products such as milk and gelatin. The concentration varies depending on the cut of meat and preparation method. Offal, including sausages encased in animal intestines, may contain higher levels of the allergen.
Jeremy had eaten beef sausages that evening, which may have intensified his reaction. Experts note that the combination of alpha-gal exposure and physical exertion can sometimes worsen symptoms. Camping conditions, stress, and environmental factors may also influence severity.
His mother, Dr Myfanwy Webb, spoke movingly during the inquest about her son’s character and talents. She described him as kind, curious, and endlessly inventive. Jeremy loved martial arts and enjoyed repairing engines and computers. Friends remembered how he could bring neglected motors back to life with patience and skill.
The grief remains raw for his family and friends. Several of his close mates have since tattooed his name in tribute. His parents have channelled their heartbreak into advocacy, determined to raise awareness of this unusual meat allergy. They hope better understanding could prevent another family experiencing similar pain.
Professor van Nunen warns that alpha-gal syndrome is increasing globally. She attributes the rise partly to ecological change and expanding tick habitats. Warmer temperatures and shifting wildlife patterns may contribute to greater human exposure. As tick populations spread, cases of meat allergy may follow.
Prevention begins with avoiding tick bites wherever possible. Experts recommend protective clothing, insect repellent, and thorough body checks after outdoor activities. If bitten, proper tick removal is crucial to reduce further allergen exposure. Education remains central to reducing risk.
The Australasian Society of Clinical Immunology and Allergy advises individuals in tick-prone regions to seek medical advice if experiencing recurring gastrointestinal symptoms after eating meat. Screening for alpha-gal antibodies can help confirm diagnosis. Early identification allows patients to modify diets and carry emergency adrenaline injectors.
Jeremy’s case has prompted renewed discussion among clinicians in Australia and beyond. It highlights the need for greater awareness of delayed allergic reactions. It also underscores the importance of considering anaphylaxis alongside asthma in sudden respiratory emergencies.
For UK readers, the story carries broader relevance. Ticks are present in parts of Britain, particularly rural and wooded areas. While alpha-gal cases remain rare in the UK, global travel and environmental shifts may influence patterns. Vigilance and informed healthcare can make a critical difference.
Jeremy Webb’s death stands as a profound reminder of nature’s unpredictable risks. A simple tick bite, once dismissed as minor, can carry unexpected consequences. His family’s courage in seeking answers has brought clarity to a complex medical puzzle.
As awareness grows, doctors hope earlier diagnosis will save lives. Families in tick-prone areas are urged to recognise unusual symptoms after eating meat. Through education and prevention, experts believe further tragedies can be avoided.
Jeremy’s legacy now extends beyond his community. His story is shaping medical understanding of meat allergy worldwide. In sharing their loss, his parents have given meaning to unimaginable sorrow.