Published: 08 January 2026. The English Chronicle Desk. The English Chronicle Online.
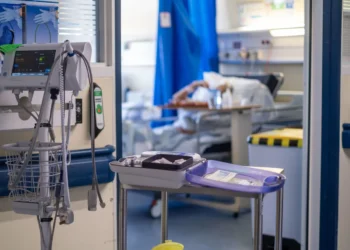
Patients collapsing in NHS corridors is becoming an increasingly serious safety issue, the watchdog warns. The Health Services Safety Investigations Body (HSSIB) revealed that overcrowding in hospitals is forcing patients into corridors, gyms, and storerooms, leaving them unseen by staff. This hidden placement can delay critical treatment and puts patients at increased risk of falls, infections, or oxygen deprivation. HSSIB’s report stressed that staff often cannot monitor these patients effectively, raising concerns about emergencies going unnoticed until it is too late.
The report highlighted multiple incidents where patients collapsed in temporary care areas, including trolleys left at corridor ends. Staff explained that some patients in these overflow areas had not been properly assessed or had treatment started, meaning deterioration may go unnoticed or detected late. Nurses emphasized that calling for emergency assistance is difficult when patients are out of the central view, creating avoidable risks.
Hospitals are trying different strategies to improve safety in corridor care. Some have installed emergency call bells, mini nursing stations, and plug sockets for medical equipment, creating calmer, more organised environments. However, other trusts avoid these measures to prevent temporary care from becoming standard practice. Despite these interventions, some patients remain in overflow areas for several days, even though the intended time is less than an hour.
The Royal College of Nursing described the HSSIB findings as a “damning indictment” of routine corridor care, warning that patients’ lives are at stake. Similarly, the Royal College of Emergency Medicine estimated that over 16,600 people died last year in England due to delays in finding a proper hospital bed after arriving at A&E.
NHS England stated that corridor care is “unacceptable and should never be considered standard,” while Health Secretary Wes Streeting promised to eliminate this practice by 2029. Staff groups remain sceptical, citing ongoing pressures and limited resources. A Department of Health spokesperson added that no patient should be cared for in corridors and emphasised ongoing efforts to improve discharge processes, data collection, and social care collaboration.
The watchdog’s report also drew attention to how patients in temporary care environments face delayed attention during medical emergencies. Some hospitals have proactively improved monitoring, but gaps remain. The presence of patients in overflow areas highlights the growing challenge NHS trusts face in balancing capacity with patient safety. Staff dedication is praised, yet structural solutions remain critical to prevent further incidents.
Experts argue that corridor care reflects deeper systemic challenges, including bed shortages and growing patient demand. Without significant investment and operational change, patients will continue to experience unsafe care in hidden areas. The HSSIB findings underscore that patient safety must remain the NHS’s top priority.
Patients collapsing in NHS corridors is therefore more than an isolated issue; it is a symptom of wider systemic strain. Ensuring proper monitoring, rapid response capabilities, and maintaining dignified care environments is essential. While the NHS works toward long-term solutions, the immediate risks to patient safety demand urgent attention and nationwide strategy.