Published: 24 November 2025. The English Chronicle Desk. The English Chronicle Online.
A critical shortage of paediatric pathologists is forcing bereaved parents to endure months of agonising waits to learn the cause of their child’s death. Families who have lost children are reporting “harrowing” delays, with one in five now waiting six months or more for post-mortem results, according to the Royal College of Pathologists (RCPath).
The shortage has been described as a crisis by the RCPath, which warns that it is not only prolonging grieving for families but also delaying vital diagnoses and treatment for foetuses, babies, and children. The organisation stressed that the lack of qualified NHS staff capable of performing post-mortem examinations is behind these delays, rather than any drop in demand for such services.
In a report published this month, RCPath highlighted that there has been “no growth in the number of paediatric and perinatal post-mortem examinations” over the last five years. The report emphasised that families continue to experience extended waits, and the workforce shortage is now at a level that the service is unable to cope effectively with current demand.
Dr Clair Evans, chair of RCPath’s advisory committee on prenatal, perinatal, and paediatric pathology, explained that these delays are deeply distressing. She said: “Our service is in crisis. Families are regularly reporting long and harrowing waits for post-mortem reports, which is simply unacceptable.” She added that some families now face waits of twelve months or more, creating enormous emotional strain for parents already grieving the unimaginable loss of a child.
According to Dr Evans, the shortage has left pathologists themselves “stretched, stressed, and burnt out,” unable to provide the high-quality care their patients deserve. Many specialists have expressed concern that the pressure of managing heavy workloads is taking a severe personal and professional toll. She said: “Due to the severe resource issues, paediatric and perinatal pathologists tell us their inability to provide high-quality care to their patients is leaving them feeling stretched, stressed, and burnt out.”
The report also revealed a geographic disparity in the availability of specialists, noting that there are no paediatric or perinatal pathology consultants in regions such as the South West, the Midlands, or Northern Ireland. This uneven distribution has exacerbated delays for families living outside major metropolitan areas, forcing some to travel long distances or wait even longer for examinations to be carried out.
RCPath has recommended immediate funding for up to thirty-seven new training posts by 2030, alongside additional resources for advanced training programmes. The organisation also called for dedicated time to allow current consultants to train the next generation of pathologists, emphasising that building capacity will require sustained investment and strategic workforce planning.
Dr Bernie Croal, president of RCPath, highlighted the urgency of the situation, urging government action across the UK. “Commitment from all four UK Governments is vital, as is investment in paediatric services,” she said. “Families should not have to endure prolonged waits after the unthinkable loss of a child. The system must be strengthened immediately.”
The Department of Health and Social Care responded, acknowledging the distress caused by delays and emphasising the government’s long-term commitment to expanding the workforce. A spokesperson said: “Bereaved parents have experienced the unthinkable and any avoidable distress to families in this heartbreaking position is unacceptable.” They added that the NHS currently has a record number of doctors across almost every specialty, including pathology, and that the 10-Year Health Plan commits to the creation of 1,000 new specialty training posts, with a focus on areas of greatest need.
Families affected by the shortage have shared their experiences of prolonged waiting periods, describing the emotional toll of not knowing why their child died. One mother, who requested anonymity, explained that she waited eight months for her son’s post-mortem report. “You feel stuck in limbo,” she said. “Every day is filled with questions you cannot answer. You are desperate for closure, and it doesn’t come. It’s a constant, heart-wrenching torment.”
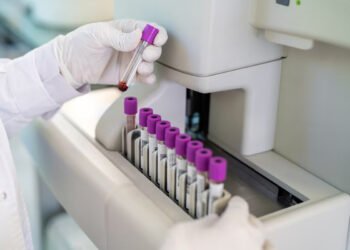
Experts say that post-mortem examinations for children and foetuses are not only essential for providing families with closure but are also critical for public health. They can help detect rare medical conditions, inform future care for other children, and contribute to research that may prevent similar deaths in the future. Paediatric pathologists, however, warn that the shortage is leaving them unable to meet these demands efficiently.
RCPath data indicates that, while demand for post-mortem examinations has remained high, workforce numbers have stagnated due to limited training capacity and difficulty recruiting specialists. The combination of an ageing workforce and a slow pipeline of new consultants has left services under unprecedented pressure. Consultants report that their caseloads are increasing, with fewer hands to manage complex cases that require highly specialised knowledge.
The shortage has also raised concerns about the potential for delayed diagnoses in live children. With fewer paediatric pathologists available, hospitals may struggle to identify underlying medical conditions in a timely manner, potentially impacting treatment outcomes. “When there are delays in pathology, there are delays in everything else,” said Dr Evans. “This can affect clinical decisions, family counselling, and long-term care planning.”
Families, charities, and professional organisations are calling for urgent reforms. Proposals include increasing training opportunities, offering incentives to attract new talent to paediatric pathology, and ensuring that existing staff are supported with adequate resources and manageable workloads. Advocates stress that without such measures, families will continue to endure unnecessary suffering, and the NHS’s ability to provide high-quality paediatric care will remain compromised.
Dr Croal added: “The NHS cannot continue to operate with this shortage. It is unacceptable that parents who have suffered the loss of a child must wait months for answers. We need immediate investment, workforce planning, and political commitment to ensure paediatric and perinatal pathology services are safe, reliable, and compassionate.”
Some parents have shared the ways in which they cope with the emotional burden while waiting. Support groups, counselling services, and charitable organisations like Child Bereavement UK and Sands provide essential guidance, but staff warn that these cannot replace timely pathology services. They emphasise that policy interventions are the only long-term solution to systemic delays.
The RCPath report concluded that urgent action is required to prevent the crisis from worsening. With an ageing population, rising healthcare demands, and increasingly complex medical cases, the shortage of paediatric pathologists is likely to become more acute unless sustained investment is made. The report urged all four UK governments to collaborate on funding, training, and workforce planning to address the shortage comprehensively.
The story of families waiting months for post-mortem results reflects the broader challenges facing the NHS. While hospitals have been dealing with pressures in staffing, funding, and service delivery, highly specialised services like paediatric pathology often receive less public attention. Yet the consequences of these shortages are deeply personal, affecting grieving families in profound ways.
Healthcare experts argue that addressing this shortage requires a multi-faceted approach, including increasing trainee numbers, improving recruitment incentives, and providing mental health support for overworked consultants. Without immediate intervention, the RCPath warns that families will continue to face harrowing waits and the NHS risks undermining public trust in critical paediatric services.
As bereaved parents struggle for answers, the call for urgent reform has never been louder. RCPath emphasises that delivering high-quality paediatric and perinatal pathology services is not only a matter of professional responsibility but a moral imperative. The hope is that with proper investment, policy reform, and support for the workforce, no family will have to endure unnecessary months of uncertainty about the loss of a child.