Published: 03 March 2026. The English Chronicle Desk. The English Chronicle Online.
Weight-loss drugs could soon change how doctors treat heart attack patients across the United Kingdom. A new UK study suggests these medicines may prevent dangerous complications after cardiac emergencies. Researchers found that weight-loss drugs might reduce tissue damage that follows blocked arteries. The findings offer fresh hope to thousands recovering from heart attacks each year. Around 100,000 people in the UK suffer a heart attack annually. Many survive thanks to rapid hospital treatment and improved emergency care. Yet up to half develop a complication that threatens long-term survival. The study indicates weight-loss drugs may lower this hidden risk significantly.
The research was funded by the British Heart Foundation and involved leading academic institutions. Scientists from University of Bristol worked alongside colleagues at University College London. Their findings were published in the respected journal Nature Communications. The results are based on laboratory and animal model investigations. Further trials in human patients will be essential before clinical use.
The complication at the centre of this discovery is known as no-reflow. It occurs even after surgeons reopen the blocked coronary artery. In these cases, blood still fails to reach parts of the heart muscle. Tiny vessels inside the heart remain constricted despite emergency intervention. This reduced circulation can cause additional tissue injury. Patients with no-reflow face higher risks of heart failure. They are also more likely to be readmitted to hospital. In severe cases, the condition increases the chance of death within a year.
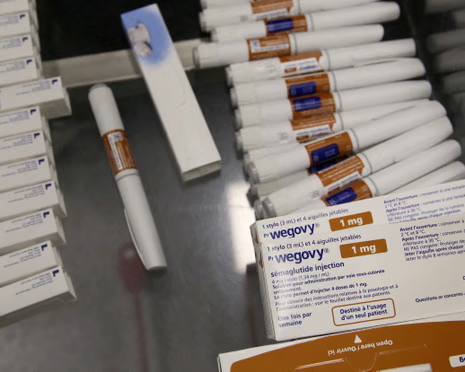
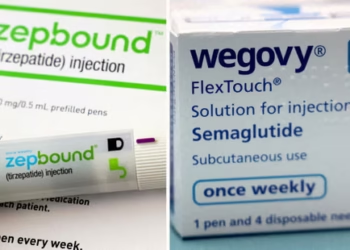
Drugs such as Ozempic and Wegovy were central to the investigation. These medications belong to a class called GLP-1 receptor agonists. They were originally developed to manage type 2 diabetes. Over recent years, they gained popularity for treating obesity. Large clinical trials have already shown cardiovascular benefits. Patients taking them experienced fewer heart attacks and strokes. However, scientists did not fully understand the protective mechanisms involved.
Dr Svetlana Mastitskaya, the study’s lead author, described the results as encouraging. She explained that nearly half of heart attack patients experience no-reflow. According to her findings, GLP-1 drugs may prevent this complication. The team observed improved microvascular blood flow in treated subjects. This effect appeared to reduce tissue injury after arterial reopening. The discovery suggests these medicines may do more than support weight management.
Professor David Attwell, who co-led the study, highlighted the potential significance. He said the drugs might offer a life-saving approach. By protecting the smallest blood vessels, they could improve recovery outcomes. This possibility has attracted attention across the cardiology community. Experts believe it may represent a new therapeutic pathway.
The hormone GLP-1 naturally regulates blood sugar and appetite. The drugs mimic this hormone’s biological activity. Researchers believe this mimicry could influence microvascular function. Improved vessel relaxation may allow blood to circulate more freely. This mechanism might explain the observed reduction in no-reflow cases. Yet scientists caution that much remains unknown. Human physiology can respond differently from laboratory models.
Professor Bryan Williams, chief scientific and medical officer at the British Heart Foundation, commented carefully. He welcomed the findings but stressed the need for caution. According to him, detailed human studies are vital. Only rigorous clinical trials can confirm safety and effectiveness. Until then, routine use in emergency care remains premature.
One of the most intriguing possibilities involves paramedic intervention. Dr Mastitskaya suggested the drugs could be administered during ambulance transport. They might also be given during surgical reopening procedures. If proven safe, early delivery could maximise protective benefits. This approach would represent a significant shift in emergency cardiology practice. However, regulators would require strong evidence before approval.
Heart attack treatment has advanced dramatically over recent decades. Rapid angioplasty and clot-busting therapies save countless lives annually. Yet long-term complications still burden patients and healthcare systems. Heart failure following myocardial damage remains a serious concern. Any therapy that reduces tissue injury would have major public health value. The NHS continually seeks strategies to improve survival and recovery.
Weight-loss drugs have already reshaped conversations around obesity management. Their cardiovascular benefits have surprised many clinicians. Some studies reported reduced inflammation and improved vascular health. Others suggested favourable effects on blood pressure and cholesterol. The new research adds another potential dimension. It points toward microvascular protection during acute cardiac events.
The financial implications also merit consideration. GLP-1 medications are relatively expensive compared with older therapies. Widespread emergency use would require careful cost assessment. Policymakers would weigh clinical benefits against budget pressures. Nonetheless, preventing hospital readmissions could offset expenses. Reduced heart failure cases would ease strain on NHS services.
Patients recovering from heart attacks often face uncertainty. Even after successful procedures, anxiety about complications persists. The possibility of added protection brings cautious optimism. Cardiologists emphasise that lifestyle changes remain essential. Smoking cessation, healthy eating, and regular exercise still form the foundation of recovery. Medication complements, but does not replace, these measures.
International observers are closely monitoring the UK findings. Similar research initiatives are underway in Europe and North America. Collaboration may accelerate progress toward human trials. If confirmed, guidelines could eventually evolve. Emergency protocols might include GLP-1 therapy alongside established interventions. Such changes would reflect a broader understanding of cardiovascular biology.
Scientists also hope the discovery will stimulate further investigation. Understanding exactly how GLP-1 influences microvessels could unlock new therapies. Researchers aim to map the cellular pathways involved. Improved insight may lead to targeted treatments with fewer side effects. The study therefore represents both a clinical and scientific milestone.
For now, experts urge balanced interpretation. Animal model results do not guarantee identical human outcomes. Safety profiles must be evaluated in acute settings. Patients experiencing heart attacks often receive multiple medications simultaneously. Interactions and timing require careful study. Regulatory agencies will scrutinise every stage of development.
Despite these caveats, enthusiasm remains palpable. Cardiovascular disease continues to claim thousands of British lives annually. Innovations that enhance recovery are urgently needed. Weight-loss drugs, once viewed narrowly as metabolic treatments, may hold broader promise. Their evolving role illustrates the interconnected nature of bodily systems.
The coming years will determine whether this promise translates into practice. Large-scale clinical trials are the next essential step. Recruitment, funding, and regulatory approval may take time. Yet the groundwork has been laid by this pioneering UK research. The collaboration between Bristol and London institutions underscores national scientific strength.
Ultimately, the discovery highlights the dynamic landscape of modern medicine. Treatments designed for one condition can reveal unexpected benefits elsewhere. As evidence grows, clinicians adapt to emerging knowledge. For heart attack survivors, that adaptability could mean improved quality of life. If confirmed, weight-loss drugs may become an unexpected ally in cardiac recovery.