Published: 05 March 2026. The English Chronicle Desk. The English Chronicle Online.
Weight loss drugs may do more than reduce waistlines, according to new research. A major US study suggests these medicines could also lower addiction risks. The findings have sparked fresh debate among doctors and policymakers across the UK. Scientists examined whether popular weight loss drugs influence the brain’s reward system. Early evidence indicates they may reduce cravings linked to alcohol and narcotics. Experts stress that more trials are needed before firm conclusions can be drawn.
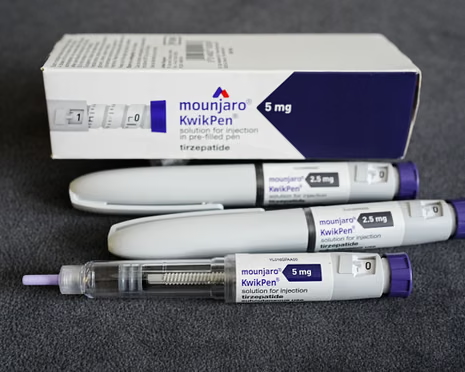
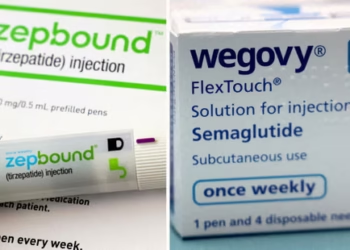
The study, published in the British Medical Journal, analysed data from 606,434 American veterans with type 2 diabetes. Researchers tracked patients for up to three years. They focused on medicines known as glucagon-like peptide-1 receptor agonists, or GLP-1s. These include widely prescribed brands such as Mounjaro and Ozempic. Both are used to manage diabetes and support significant weight reduction.
Scientists found that patients taking GLP-1 medicines showed lower rates of substance misuse. Among those with no previous addiction history, alcohol-related disorders fell by 18 percent. Cannabis use declined by 14 percent. Cocaine and nicotine use each dropped by 20 percent. Opioid misuse showed the largest reduction at 25 percent. These outcomes were compared with patients prescribed other diabetes treatments.
The research also revealed striking results among patients already using illicit substances. Those on GLP-1 therapies experienced 39 percent fewer overdoses. Emergency hospital visits fell by 31 percent. Most notably, the risk of death from substance use dropped by 50 percent. Such figures have drawn attention from addiction specialists worldwide.
GLP-1 medicines mimic a hormone released naturally after eating. This hormone helps regulate blood sugar and promotes feelings of fullness. However, scientists believe the drugs may also affect dopamine pathways. These pathways play a central role in reward and addictive behaviour. By influencing these circuits, the drugs could reduce cravings beyond food.
Professor Claire Anderson, president of the Royal Pharmaceutical Society, described the findings as promising yet preliminary. She explained that the study was observational in nature. Therefore, it cannot prove that the medicines directly prevent addiction. She emphasised the need for controlled clinical trials to establish causation.
Her caution reflects broader scientific consensus. Observational studies can reveal associations but not definitive proof. Patients prescribed GLP-1 drugs may differ in lifestyle or healthcare access. Such factors could partly explain the reduced addiction rates. Nevertheless, researchers argue that the scale of the data strengthens the credibility of results.
Interest in weight loss drugs has surged dramatically over the past two years. Social media platforms are filled with personal transformation stories. At the same time, concerns have emerged about side effects and long-term sustainability. Nausea, vomiting, and digestive discomfort remain common complaints. Costs can also be significant, particularly for private prescriptions.
In the UK, access through the NHS has expanded gradually. However, pharmacy leaders say the rollout remains slow. Gareth Jones of the National Pharmacy Association called the study significant. He suggested that weight loss drugs may offer broader health benefits. Obesity continues to place immense strain on NHS services nationwide.
Beyond addiction, researchers are examining cardiovascular and metabolic impacts. Some evidence already shows reduced risks of heart disease. The potential mental health implications now add another dimension. Addiction services in Britain face rising demand and limited resources. Any treatment that lowers overdose risk could ease pressure.
Yet optimism is tempered by findings from a separate Cambridge-led review. Experts at the University of Cambridge analysed 48 previous studies. Their meta-analysis appeared in the journal eClinical Medicine. It found that many patients regain most lost weight after stopping medication. Within a year, individuals typically regained around 60 percent of shed weight.
Over longer periods, weight regain reached 75 percent on average. Researchers concluded that only 25 percent of initial weight loss tends to be sustained. For someone who lost 20 percent of body weight, that equates to a lasting five percent reduction. The findings highlight the chronic nature of obesity management.
Adherence also poses challenges. Around half of users discontinue GLP-1 treatment within one year. After two years, approximately three-quarters have stopped entirely. Side effects and financial burden often drive this trend. Experts warn that stopping suddenly may reverse metabolic improvements.
Public perception further complicates the picture. A survey by Simple Online Pharmacy questioned more than 3,000 users. Two-thirds said they concealed their medication use from friends or family. Many feared judgment or accusations of taking shortcuts. Among those criticised, most were told simply to eat less and exercise more.
Such stigma reflects persistent misunderstandings about obesity. Medical professionals increasingly describe it as a complex chronic disease. Genetics, environment, and hormonal regulation all play roles. Weight loss drugs target biological pathways, not personal willpower. The emerging addiction findings may reinforce that scientific perspective.
Addiction specialists are watching developments carefully. Substance misuse remains a serious issue across Britain. Alcohol-related hospital admissions continue to burden emergency departments. Drug-related deaths in parts of England and Scotland remain among Europe’s highest. Any therapy that reduces overdose risk commands attention.
However, experts caution against oversimplified headlines. Weight loss drugs are not currently licensed for treating addiction. Prescribing them for this purpose would require robust evidence. Randomised controlled trials would need to confirm safety and effectiveness. Regulators would also examine potential unintended consequences.
There are ethical considerations too. Expanding indications could increase already intense demand. Supply shortages have affected diabetes patients in recent months. Policymakers must balance innovation with equitable access. The NHS faces financial constraints and competing priorities.
Despite uncertainties, researchers remain intrigued by the biological mechanisms involved. The overlap between appetite control and reward processing offers fertile ground. Some neuroscientists argue that addiction and overeating share similar circuitry. If GLP-1 medicines modulate that circuitry, broader therapeutic uses may emerge.
For now, clinicians advise patients to follow approved guidelines. Those prescribed GLP-1 drugs should use them under medical supervision. Lifestyle support remains essential for sustained results. Addiction treatment continues to rely on counselling, medication, and community services.
The conversation surrounding weight loss drugs is evolving rapidly. What began as a breakthrough in diabetes care now touches mental health and addiction science. British experts emphasise careful interpretation of early data. Yet they also acknowledge the importance of exploring innovative solutions.
As research progresses, policymakers will face complex decisions. Balancing access, affordability, and evidence will prove challenging. Patients, meanwhile, seek treatments that address interconnected health issues. The possibility that one medicine could tackle both obesity and addiction is compelling.
Ultimately, science advances through cautious optimism. The new findings illuminate intriguing pathways between metabolism and behaviour. Whether weight loss drugs become part of addiction therapy remains uncertain. What is clear is that the debate has entered a new phase.