Published: 30 January 2026. The English Chronicle Desk. The English Chronicle Online.
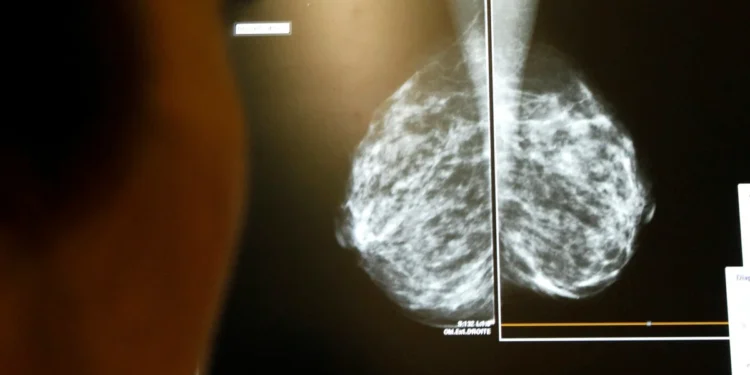
Artificial intelligence is increasingly reshaping modern medicine, and new evidence suggests it could transform early cancer detection. A major international study has found that AI breast screening significantly reduces the likelihood of women receiving a later-stage cancer diagnosis. The research indicates a measurable improvement in early detection, alongside a reduction in aggressive cancers that often require intensive treatment. For healthcare systems under pressure, the findings highlight how carefully integrated technology may support clinicians without replacing human expertise.
The study, described by researchers as the first trial of its scale, examined the impact of AI breast screening within routine mammography services. Conducted in Sweden, it involved around 100,000 women who attended scheduled breast screening appointments. Participants were randomly allocated either to traditional mammogram readings performed by two radiologists or to an AI-supported system that assisted clinical decision-making. The trial ran from April 2021 until December 2022, offering a substantial data set for analysis.
At the heart of the research was a sophisticated AI tool designed to analyse mammogram images before human review. The system categorised scans into risk levels, assigning low-risk images to a single radiologist and directing high-risk cases for double reading. Suspicious areas were highlighted to draw clinical attention, enabling radiologists to focus their expertise where it mattered most. This approach aimed to maintain safety while easing workload pressures in overstretched screening services.
Results published in The Lancet revealed that mammography supported by artificial intelligence led to a 12% reduction in cancer diagnoses during the years following screening. In numerical terms, 1.55 cancers were diagnosed per 1,000 women in the AI-supported group, compared with 1.76 per 1,000 in the standard screening group. Researchers interpret this difference as evidence that more cancers were identified earlier, reducing the number emerging later at more advanced stages.
Early detection is a critical factor in breast cancer outcomes, and the study demonstrated clear progress in this area. More than 81% of cancers in the AI-supported group were detected during routine screening appointments. By contrast, just under 74% were identified at the screening stage in the control group. This improvement suggests that AI breast screening can help identify tumours before symptoms develop, when treatment options are often less invasive and more effective.
Another striking finding concerned aggressive cancer subtypes, which tend to grow quickly and spread faster. The AI-supported group experienced nearly 27% fewer aggressive cancers than those receiving standard screening. While researchers caution that longer-term follow-up is needed, the data indicates that earlier detection may prevent some aggressive cancers from progressing unchecked between screenings.
Dr Kristina Lång of Lund University, the study’s lead author, described the results as encouraging but emphasised the need for careful implementation. She noted that AI-supported mammography could help detect cancers at an earlier stage while also reducing the workload for radiologists. However, she stressed that healthcare systems must introduce AI cautiously, using tools that are thoroughly tested and continuously monitored.
According to Dr Lång, the technology should not be viewed as a replacement for clinicians but as a support mechanism. Radiologists remain essential for interpreting results, making clinical judgments, and communicating with patients. The study itself required at least one human reader for every mammogram, reinforcing the idea that AI breast screening works best as a partnership between technology and medical expertise.
Breast cancer remains one of the most significant health challenges facing women worldwide. Globally, more than two million people are diagnosed each year, and it is a leading cause of death among women aged 35 to 50. Early diagnosis is strongly linked to survival rates, making improvements in screening accuracy particularly valuable for public health.
Despite the promising results, experts urge caution before widespread adoption. Dr Sowmiya Moorthie, a senior strategic evidence manager at Cancer Research UK, welcomed the findings but highlighted limitations. She explained that while AI-assisted readings can improve efficiency, there is ongoing concern about the risk of missed cancers. This single-centre study provides reassurance, she said, but further research across different populations and healthcare systems is essential.
Dr Moorthie added that rising cancer rates will place increasing strain on services like the NHS. Innovations such as AI breast screening could play a vital role in addressing these pressures. However, she emphasised that any new technology must undergo rigorous evaluation to ensure it genuinely benefits patients and does not introduce unintended harms.
Charities focused on breast cancer research and advocacy have also responded positively. Simon Vincent, chief scientific officer at Breast Cancer Now, said the trial underlined the enormous potential of artificial intelligence in screening programmes. He noted that screening is one of the most effective tools for detecting breast cancer early, and earlier diagnosis is closely linked to improved survival chances.
Vincent highlighted that UK trials launched recently are already exploring how AI might be safely integrated into NHS breast screening. These studies will be crucial in determining best practice, ensuring patient safety, and establishing how such tools can be deployed at scale. The Swedish findings provide a strong evidence base to support continued investigation within the UK context.
From a health policy perspective, the study raises important questions about workforce planning and resource allocation. Radiology departments across Europe face staff shortages, increasing workloads, and growing demand. AI breast screening systems that safely reduce reading volumes could help clinicians focus on complex cases, improving efficiency without compromising care standards.
However, researchers agree that technology alone cannot solve systemic challenges. Successful implementation requires investment in training, robust governance frameworks, and clear accountability structures. Continuous data monitoring is essential to ensure that AI tools perform consistently across diverse populations and over time.
Patients’ trust will also play a crucial role in adoption. Transparency about how AI systems are used, how decisions are made, and how human oversight is maintained will be key to public acceptance. The Swedish study demonstrates that when used responsibly, artificial intelligence can enhance, rather than undermine, confidence in screening programmes.
Looking ahead, longer-term follow-up will determine whether earlier detection through AI breast screening translates into reduced mortality. While fewer late-stage diagnoses and aggressive cancers are encouraging indicators, survival outcomes remain the ultimate measure of success. Researchers plan continued monitoring to assess these critical endpoints.
For now, the findings represent a significant step forward in understanding how artificial intelligence can support cancer prevention strategies. They suggest that with careful oversight, AI can strengthen existing healthcare systems and deliver tangible benefits for patients. As further trials progress in the UK and beyond, evidence from studies like this will shape the future of breast cancer screening.