Published: 27 February 2026. The English Chronicle Desk. The English Chronicle Online.
The debate over health funding between the United States and several African nations has intensified, stirring deep unease across the continent’s political and public health landscape. Zimbabwe’s decision to withdraw from talks on a significant bilateral health aid package underscored growing resistance to what critics describe as unequal and intrusive terms. The dispute has drawn diplomatic criticism, legal challenges, and fresh scrutiny from regional health authorities who argue that new agreements compromise sovereignty and community interests for substantial funding.
Zimbabwe’s formal rejection of a proposed health aid arrangement worth hundreds of millions of dollars was framed by its leaders as a necessary defence of national autonomy and public health governance. President Emmerson Mnangagwa’s administration said the negotiating terms, which reportedly included extensive data access provisions, risked making Zimbabwe too dependent on foreign guidance for the management of sensitive health information. Authorities argued that powerful nations should not extract biological data without guaranteed reciprocation in access to vaccines or treatments.
The government’s stance reverberated across diplomatic circles, with officials emphasising that any agreement must respect Zimbabwe’s ability to make independent decisions about its health priorities. This position aligns with broader concerns that the new generation of health partnerships promoted by Washington under its “America First” health strategy constitutes a departure from traditional multilateral cooperation. Zimbabwe’s withdrawal from negotiations has raised questions about the future of U.S. funding that has long supported the country’s HIV and tuberculosis programmes.
Elsewhere, Zambia has also voiced significant reservations about the structure of a planned U.S. health funding deal, which was due to include more than one billion dollars in support. The agreement, intended to tackle HIV, malaria, maternal and child health issues, and disease preparedness, has stalled after Zambian officials said parts of the proposal did not align with their national interests. Reacting to media scrutiny of the draft pact, government representatives asked for revisions and greater clarity on provisions linked to unrelated sectors like mining collaboration and data management.
Civil society groups in Zambia and beyond have expressed alarm at elements they believe could prioritise external strategic interests over local community health needs. Health advocates warned that conditional funding tied to economic concessions or long‑term data access commitments could undermine the integrity of domestic healthcare systems and divert attention from core health challenges. Critics also highlighted a lack of transparency in negotiations, suggesting deeper engagement with community groups and health professionals was urgently needed.
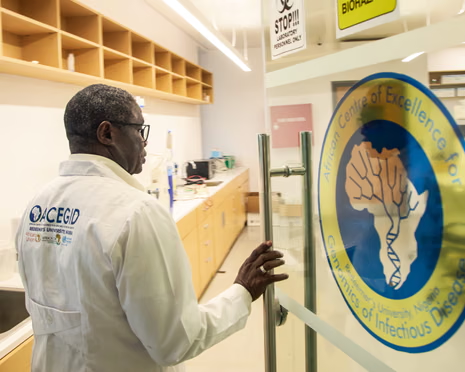
The Africa Centres for Disease Control and Prevention has entered the debate, with its director general raising public concerns about how some bilateral agreements require the sharing of critical health data, including pathogen information, as a precondition for receiving funding support. At a virtual press briefing, the agency’s head questioned whether such requirements could expose African health systems to undue risk and complicate responses to future outbreaks. This feedback added a regional health governance perspective to the ongoing diplomatic dialogue.
In Kenya, the unfolding situation has taken a legal turn as civil organisations brought a case challenging the constitutionality of agreements signed with the United States. A High Court temporarily suspended implementation after campaigners argued that the data sharing terms contravened national privacy protections. The outcome of this case is being watched closely across the continent, as it could set important legal precedents regarding how sovereign nations engage with powerful external partners on health matters.
At the heart of these disputes lies a fundamental philosophical divide about how health assistance should be structured. Washington’s approach departs from the historic model led by entities such as the World Health Organization and the now‑dismantled United States Agency for International Development, focusing instead on direct bilateral partnerships that require increasing contributions from recipient governments over time. Proponents of this model argue it promotes self‑reliance and ensures that each country has a seat at the negotiating table.
Supporters of the new strategy also contend that the scale of funding on offer cannot be ignored. Nations negotiating or signing agreements with the United States are often facing severe health system challenges that would otherwise go unfunded. For example, the Democratic Republic of Congo recently agreed to a $1.2 billion health partnership intended to strengthen disease surveillance and resilience against infectious threats. This deal, while controversial, illustrates how some governments are willing to engage in these bilateral frameworks to secure long‑term support.
 Still, sceptics caution that tying aid to terms perceived as one‑sided could erode trust and deepen dependency, even if increased domestic funding obligations are part of the framework. Public health advocates emphasise that genuine partnership must be rooted in mutual respect, clear benefit sharing, and robust safeguards for patient privacy. Without these elements, they argue, there is a risk of creating structural inequities under the guise of cooperation.
Still, sceptics caution that tying aid to terms perceived as one‑sided could erode trust and deepen dependency, even if increased domestic funding obligations are part of the framework. Public health advocates emphasise that genuine partnership must be rooted in mutual respect, clear benefit sharing, and robust safeguards for patient privacy. Without these elements, they argue, there is a risk of creating structural inequities under the guise of cooperation.
From Harare to Lusaka and Nairobi, the debates reflect broader questions about how international health diplomacy should evolve in a post‑pandemic world. African leaders asserting their sovereignty argue that health funding must support national priorities without compromising control over sensitive information or yielding undue leverage to external partners. These concerns echo in international forums and are shaping how negotiations proceed.
As Africa navigates these complex negotiations, the reactions reveal a nuanced interplay between securing essential health resources and safeguarding sovereign decision‑making. Governments and civil society alike are pushing for more equitable terms that uphold ethical standards while addressing the urgent health needs of their populations. Observers note that the outcome of these debates could influence wider global health funding practices for years to come.
In the meantime, some countries are advancing cautiously, seeking assurances that their data, biological samples, and strategic health information will be protected and used in ways that benefit their communities. Emerging legal challenges, regional health authority involvement, and heightened public scrutiny are shaping this contentious chapter in global health relations. The results of these negotiations will likely resonate far beyond the immediate stakeholders, affecting how the global community approaches collaboration, data governance, and equitable access to medical advancements in the years ahead.