Published: 06 May 2026. The English Chronicle Desk. The English Chronicle Online.
The landscape of public health in England currently faces a deeply concerning and urgent challenge. Recent findings have revealed a significant divide in how different communities experience life-threatening medical emergencies. People from black backgrounds in England are now twice as likely to suffer from strokes. This data comes from the largest and most comprehensive study ever conducted on the specific subject. Researchers from King’s College London presented these findings at the European Stroke Organisation conference this week. Their analysis covered thirty years of data from the renowned South London Stroke Register records. This register is unique because it tracks every single stroke within a very specific area. It offers a much more accurate picture than standard clinical trials which use selected participants. The study looked at a population of over three hundred thousand people over several decades. During this time researchers identified more than seven thousand individual cases of stroke within London. Stroke rates actually fell significantly between the late nineties and the early two thousand and tens. However the data shows a worrying thirteen percent rise in cases over the last four years. This recent increase has not affected all ethnic groups in the same way across the country. People of black African and Caribbean heritage are facing a much higher risk than white residents. The incidence rate is over one hundred percent higher for those with black African family roots. Those from black Caribbean backgrounds face a risk that is exactly double that of white people.
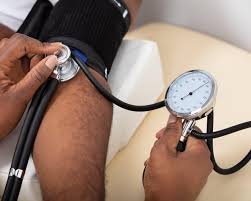
These statistics highlight a growing health inequality that demands immediate attention from the national government. High blood pressure is a primary driver of these statistics within the affected black communities today. People from black backgrounds are nearly fifty percent more likely to suffer from high blood pressure. They are also twice as likely to live with diabetes compared to their white English neighbors. These risks persist even when researchers account for different levels of wealth and social status. Dr Camila Pantoja-Ruiz led the research team and offered some vital context for these figures. She suggested the recent spike might be a lasting shadow cast by the global pandemic period. Access to primary care and regular blood pressure monitoring decreased sharply during the various lockdowns. These disruptions hit black and deprived communities much harder than other areas of the United Kingdom. Dr Pantoja-Ruiz also pointed toward broader systemic issues that influence these very different health outcomes. Factors like racism and unconscious bias can subtly affect the quality of care patients receive daily. Socioeconomic circumstances also play a massive role in how easily people can access medical support services. The study specifically highlighted intracerebral haemorrhage as a major concern for these specific patient groups. This type of stroke is linked very strongly to blood pressure that is not controlled. High blood pressure remains far more common in black communities across major cities in the country.
The disparities do not end once a patient has been admitted to a local hospital. Survival is only the first step in a very long journey toward a full recovery. The study found that black African survivors are much less likely to receive necessary follow-up care. Specifically they are thirty-four percent less likely to get the NHS support they need after discharge. Timing is another tragic factor as black patients suffer strokes much earlier in their lives too. On average these individuals are falling ill ten to twelve years sooner than white patients are. This means that people are being hit by life-changing conditions during their most productive years. The period immediately following a stroke is the most critical time for preventing a second occurrence. Without proper follow-up care patients are left extremely vulnerable to further and more severe health problems. Dr Pantoja-Ruiz noted that a lack of trust in the healthcare system plays a role. This mistrust often stems from historical and ongoing experiences of discrimination within the medical field itself. Patients may feel hesitant to engage with services that have previously failed to meet their needs. This creates a cycle where the most vulnerable people are the least likely to seek help. Solving this will require more than just medical intervention and better blood pressure medication alone. It requires a fundamental shift in how the healthcare system interacts with diverse local populations today.
Maeva May works as the director of policy at the well-known charity the Stroke Association. She expressed deep concern that stroke rates are rising again after years of steady national progress. Her organization believes that black communities are currently bearing a completely disproportionate burden of this disease. This rise is fueled by risk factors that are often undetected or are not treated well. High blood pressure causes around half of all strokes seen in the United Kingdom each year. Social and economic factors like poor housing also shape health long before a stroke occurs. When people live in stressful or inadequate conditions their physical health inevitably begins to decline. However May also emphasized that progress is possible if the right actions are taken now. Stroke rates fell for two decades because prevention programs were effective and reached many different people. The current challenge is ensuring that this vital support reaches every single community equally and fairly. The government must prioritize stroke prevention and listen to the voices of those most affected. We need a healthcare system that treats every person with the same level of urgency. This study serves as a wake-up call for policy makers and local health authorities alike. We cannot ignore the evidence that some lives are being protected better than others in England. Every citizen deserves an equal chance at a long and healthy life regardless of background. Addressing these inequalities is not just a medical necessity but also a matter of social justice. The future of the NHS depends on its ability to serve all of its patients. By focusing on targeted prevention we can start to close this dangerous and growing health gap. Together we can work toward a future where stroke risk is minimized for every single person.