Published: 14 October 2025. The English Chronicle Desk. The English Chronicle Online.
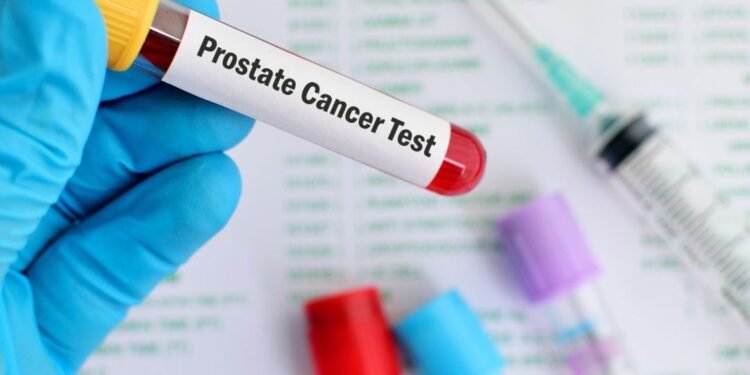
A new report suggests that targeted prostate cancer screening could save thousands of lives each year at a cost of just £18 per person, offering what experts describe as a “generational opportunity” to improve men’s health across the UK.
The findings indicate that screening men most at risk – including those who are black, have a family history of the disease, carry genes linked to prostate cancer, and are aged between 45 and 69 – could prevent thousands of deaths and add more than 1,200 years of life annually. The research, due to be presented in the House of Commons on Tuesday, also shows that expanding screening to all men aged 50 to 69 would still cost significantly less than the NHS breast cancer screening programme, which currently costs £22 per woman.
The proposal comes after long-standing debates about the effectiveness and cost of PSA (prostate-specific antigen) testing. For years, the UK National Screening Committee (UK NSC) has resisted introducing a formal screening programme, citing concerns about the reliability of PSA tests and the risk of overdiagnosis. However, recent advances in diagnostic tools, including MRI-guided testing, have strengthened the case for targeted screening by allowing clinicians to more accurately identify cases that require treatment.
Professor Calvin Bailey, chairman of the All-Party Parliamentary Group on prostate cancer, emphasised the potential impact of the proposed approach. “By targeting the men who are at highest risk, we can make the programme extremely cost-effective while saving lives that would otherwise be lost to this devastating disease,” he said. The research estimates that targeted testing would cost roughly £20,000 for every year of life saved, a figure well within the thresholds usually considered cost-effective for NHS interventions.
Former Prime Minister Rishi Sunak, who has publicly called for the introduction of targeted screening, welcomed the report’s findings. “This report makes clear that a targeted screening programme for prostate cancer is deliverable and would save lives,” Sunak said. “The screening committee should now seize this chance to make a generational impact on men’s health, deliver the preventative care our country needs, and give thousands of families more precious years together.”
The report will be officially launched at a reception in Westminster, with Sunak, Deputy Prime Minister David Lammy, and Bailey in attendance. Lammy, who has personal experience with the disease in his own family, highlighted the urgency of the issue. He revealed last year that three of his uncles and his brother had prostate cancer, and he himself faced a prostate scare before the last general election. “Because of my own ethnic profile, and because of these instances in my own family, it was a little bit hairy and a little bit scary,” he said, adding that targeted screening could provide reassurance and save lives for men facing similar risks.
Statistics underline the pressing need for action. Prostate cancer is the most common cancer in men in the UK, with approximately 67,000 new diagnoses and 12,000 deaths annually. Men of Black African or Caribbean heritage are twice as likely to develop the disease and face significantly higher mortality rates, while a family history or certain genetic factors can also sharply increase risk. Campaigners argue that the current reliance on opportunistic testing – where men must request a PSA test from their GP – leaves many at high risk without adequate protection, particularly in deprived areas where uptake is lowest and death rates are often highest.
Charities and health experts have also pointed to the evolving scientific evidence supporting screening. Modern diagnostic pathways allow for more precise use of MRI scans and biopsies, reducing the likelihood of overdiagnosis and unnecessary treatment, a central concern in previous UK NSC assessments. The report notes that a modest increase of around 23 per cent in PSA tests, MRIs, and biopsies would be sufficient to accommodate the targeted screening programme. The workforce implications are minimal, requiring only a 0.01 per cent increase in GP numbers, a 0.4 per cent increase in pathologists, and five additional MRI machines nationally.
Cost considerations further strengthen the case for action. Offering targeted checks to around 1.4 million high-risk men every five years would amount to roughly £25 million, while saving an estimated 1,254 years of life annually. Expanding the programme to include all men aged 50 to 69 would still be cheaper than the NHS breast cancer screening programme, at a projected cost of £144 million compared with £199 million for breast checks. The report describes these costs as “modest” and within reach of the NHS, especially given the potential health gains and prevention of late-stage cancer treatments, which are far more expensive and resource-intensive.
The political dimension of the debate is significant. With the UK NSC set to report next month, charities and campaigners are pressing the government to take decisive action, arguing that failure to implement a screening programme would perpetuate preventable deaths. Prostate Cancer Research and other organisations point to international examples, noting that countries such as the United States and parts of Europe have successfully integrated PSA testing into national screening strategies, particularly for high-risk populations.
Critics have historically raised concerns that screening might lead to overdiagnosis, unnecessary biopsies, and anxiety for men who test positive for PSA elevations that do not indicate aggressive cancer. However, the new report argues that advances in imaging and follow-up protocols effectively address these risks, making a targeted approach both safe and clinically beneficial.
The discussion also touches on health inequalities. Uptake of voluntary PSA testing is lowest in deprived communities, leaving men in these areas disproportionately vulnerable to late diagnoses. By proactively offering targeted screening, the programme could reduce disparities in outcomes and ensure that high-risk populations receive timely intervention. The report makes clear that targeted testing is both a clinically sound and socially responsible public health strategy.
Stakeholders emphasise that the window for implementation is narrow but achievable. With political support from figures such as Sunak, Lammy, and Bailey, alongside evidence-based backing from leading medical experts, the introduction of targeted prostate screening could mark a turning point in men’s healthcare in the UK. Advocates argue that inaction would represent a missed opportunity to prevent thousands of deaths and improve the quality of life for men and their families.
In summary, the report presents a compelling case for the NHS to adopt targeted prostate cancer screening for high-risk men. At just £18 per person, the programme promises to save lives, add years of life, and do so at a cost lower than many existing national screening initiatives. With improved diagnostics, modest workforce adjustments, and political will, experts say the intervention is feasible, affordable, and urgently needed. As the debate continues in the Commons, health campaigners hope that decision-makers will seize the opportunity to implement a screening programme that could have a profound and lasting impact on men’s health across the country.