Published: 17 October 2025. The English Chronicle Desk. The English Chronicle Online.
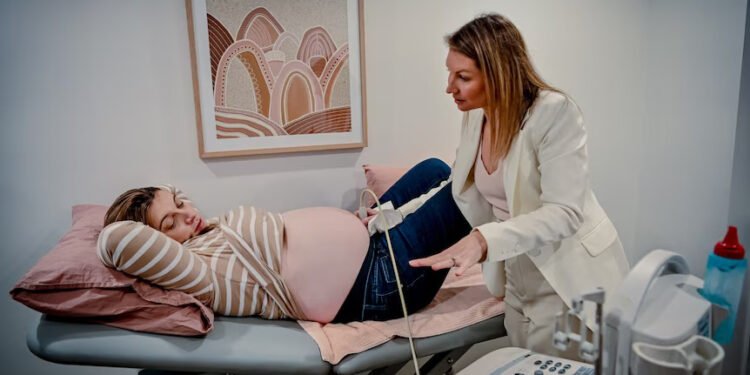
Pregnant women in England are facing a growing risk of severe injury during childbirth, according to recent NHS figures. The number of mothers experiencing third- or fourth-degree perineal tears has increased from 25 in 1,000 births in June 2020 to 29 in 1,000 in June 2025, representing a 16% rise. Such injuries can have profound and lasting effects on women’s physical and mental health, including post-traumatic stress disorder and fear of future pregnancies.
Experts link the rise in serious tears to a combination of factors, including understaffed NHS maternity units, inadequate risk assessments, and the increasing age and size of mothers. Hospitals are criticised for not consistently using recommended methods to evaluate the likelihood of perineal injuries, leaving many women at heightened risk during childbirth.
“Behind these figures are heartbreaking stories of women suffering unimaginable trauma at a moment that should be full of joy,” said Helen Morgan, the Liberal Democrat health spokesperson, who obtained the NHS data from the House of Commons library. Morgan also criticised successive governments for failing to safeguard maternal health adequately.
Almost 3% of women giving birth in England now suffer severe perineal tears, injuries that can damage the anal sphincter, causing long-term pain, incontinence, and birth trauma. The rise comes amid heightened scrutiny of NHS maternity services, prompting Health Secretary Wes Streeting to launch a national inquiry and establish a taskforce to improve care.
Poor recognition and management of severe tears contribute significantly to maternity errors, which cost the NHS over £1 billion annually. For example, University Hospitals Sussex NHS Trust agreed in August to pay £500,000 in damages to a woman who suffered lifelong complications after a fourth-degree tear was misdiagnosed at Princess Royal Hospital in Haywards Heath in 2021. The error resulted in a rectovaginal fistula, chronic pain, psychosexual difficulties, PTSD, and an inability to return to full-time work.
Third- and fourth-degree tears, known as obstetric anal sphincter injuries (OASI), affect the perineum, anal sphincter, and, in the case of fourth-degree tears, the rectum. Chloe Oliver, chief executive of the birth injury charity Mothers with Anal Sphincter Injuries in Childbirth, explained that OASI injuries are more likely during prolonged labour, first births, back-to-back babies, forceps deliveries, babies weighing over 4kg, and among mothers of Asian ethnicity. Injuries are also more common when forceps or ventouse suction devices are used.
Oliver emphasised the devastating effects of OASI, including chronic pelvic pain, urinary and faecal incontinence, difficulties with bonding and breastfeeding, psychosexual dysfunction, relationship or career breakdown, postnatal depression, anxiety, PTSD, and tokophobia—a fear of future pregnancies.
The National Maternity and Perinatal Audit report revealed that 3.29% of women giving birth vaginally in England, Scotland, and Wales in 2023 suffered some form of perineal tear. Dr Ranee Thakar, president of the Royal College of Obstetricians and Gynaecologists, noted that while most tears are minor and heal quickly, deeper tears require surgical repair and prolonged recovery.
To mitigate risk, all maternity units should implement the “OASI care bundle,” designed to assess the likelihood of severe tears. However, experts warn this protocol is not consistently followed, leaving many mothers vulnerable.
A Department of Health and Social Care spokesperson acknowledged the trauma caused by severe tears, stressing that the government has inherited a system in need of reform. They highlighted ongoing initiatives, including the national maternity investigation, taskforce, and expanded perinatal pelvic health services, aimed at reducing the incidence of perineal injuries and improving care standards across England.
As concern grows over the rising number of severe childbirth injuries, healthcare professionals, advocates, and policymakers are urging immediate action to ensure mothers can experience childbirth safely, with better risk assessment, staffing, and postnatal support. The issue has prompted wider discussions about maternity care quality, long-term health consequences, and the urgent need to prioritise maternal wellbeing across the NHS.
The NHS continues to monitor trends in perineal injuries, aiming to implement preventative measures that reduce risks for women giving birth. Awareness campaigns, training for maternity staff, and robust care protocols are being emphasised as vital steps to ensure that childbirth is safe and that mothers do not endure unnecessary trauma during one of life’s most significant moments.