Published: 30 April 2026. The English Chronicle Desk. The English Chronicle Online.
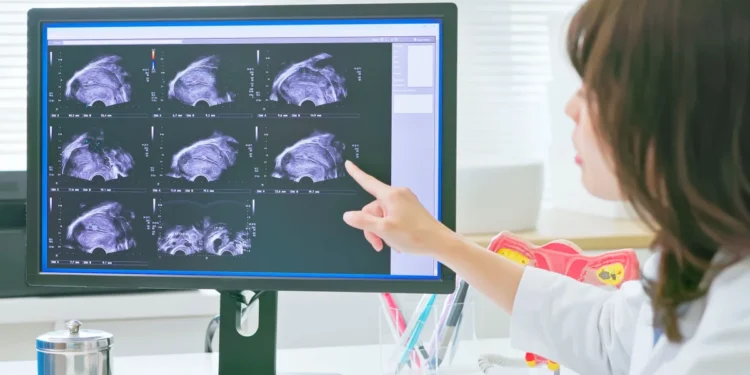
The landscape of women’s healthcare in the United Kingdom is currently facing a significant shift. For decades, thousands of women have suffered in silence due to the elusive nature of endometriosis. This chronic condition often remains hidden deep within the body for many years without proper detection. Recent clinical trials have now introduced a revolutionary non-invasive scanning technique that could change everything. This new method uses an experimental radiotracer to identify the presence of painful endometrial tissue. Experts believe this breakthrough could finally end the era of mandatory and invasive diagnostic surgeries. The trial results have sparked immense optimism among medical professionals and patient advocacy groups alike. Many hope this technology will significantly reduce the agonizingly long waiting times for a diagnosis. Currently, women in England face an average wait of nearly ten years for answers. This delay often leads to worsening physical symptoms and profound emotional distress for those affected. The trial involved a small group of nineteen women who were already seeking surgical intervention. Researchers utilized a specialized tracer called maraciclatide to highlight areas of active disease during scans. This substance specifically targets tissues that are actively forming new blood vessels within the pelvic cavity. Such activity is a hallmark sign of endometriosis that traditional scans often fail to see.
The results showed that the scans aligned with surgical findings in sixteen out of nineteen cases. Most importantly, the experimental imaging process produced no false positive results during the initial trial. Professor Krina Zondervan leads the department of women’s health at the prestigious University of Oxford. She emphasized that the most common form of this disease currently evades all reliable detection. Without this new technology, patients have no choice but to undergo risky and expensive surgery. If phase three studies confirm these findings, the impact on global clinical practice will be transformative. It would empower doctors to develop better treatments for women across the entire world today. Endometriosis occurs when tissue similar to the womb lining grows in other areas of the body. These growths typically appear on the ovaries, fallopian tubes, or the lining of the pelvis. Patients frequently report experiencing debilitating period pain and severe discomfort during daily activities like walking. The condition can also lead to painful bowel movements and significant issues with long-term fertility. Approximately one in ten women will experience these life-altering symptoms at some point in time. Despite its prevalence, the medical community has long struggled to provide quick and accurate diagnostic tools. Current treatments include hormone medications or the surgical removal of the offending abnormal tissue growths. However, the lack of early detection means many women receive treatment only after significant damage.
The charity Endometriosis UK recently highlighted the shocking disparities in current diagnosis times across England. Their research indicates that women from ethnic minority backgrounds often wait even longer for medical help. Some statistics suggest these women wait up to eleven years before receiving a formal medical diagnosis. Health Secretary Wes Streeting recently addressed these systemic failures within the government’s renewed health strategy. He noted that the progression of the disease can restrict many vital choices regarding future fertility. Early detection is therefore essential to preserving the reproductive health and well-being of young women. Peritoneal endometriosis is the earliest and most frequent subtype of this very painful chronic condition. Standard MRI scans are usually only effective at spotting structural changes in more advanced stages. This means that early-stage patients often receive clear scan results despite having very severe symptoms. The introduction of maraciclatide seeks to bridge this gap by focusing on biological activity instead. This innovative approach was developed by a UK-based biotechnology company called Serac during recent years. By binding to new blood vessels, the tracer makes the disease glow on specialized scans. This allows doctors to see exactly where the problematic tissue is located without any incisions. The nineteen participants in the study underwent a scan known as a Spect-CT after receiving infusions.
The accuracy of these scans provides a strong foundation for much larger clinical trials ahead. Serac has already announced plans to validate these promising findings through extensive phase three testing. A minimally invasive diagnostic tool would also make it easier to test new pharmaceutical treatments. Currently, researchers find it difficult to monitor how well new drugs work without repeated surgeries. A simple scan would allow for real-time monitoring of how the disease responds to medication. Dr. Tatjana Gibbons served as the lead author of the study published in the Lancet. She described the findings as a highly promising tool for both diagnosis and long-term monitoring. This is especially true for superficial peritoneal endometriosis which remains the hardest type to identify. The medical community is now calling for increased funding to bring this technology to hospitals. If successful, the NHS could see a massive reduction in the backlog for diagnostic laparoscopies. This would free up surgical resources for those who truly need operative intervention for treatment. Patients have expressed a sense of relief at the prospect of being heard sooner. For many, a quicker diagnosis means they can start managing their symptoms in their twenties. This prevents the loss of career opportunities and social connections caused by chronic pelvic pain. The psychological burden of being told your pain is normal would finally be removed forever.
The English Chronicle understands that several major UK hospitals are eager to join the next phase. These upcoming trials will involve hundreds of women to ensure the scan is truly reliable globally. Advocates argue that women’s health has been historically underfunded compared to other major medical fields. This breakthrough represents a significant step toward achieving parity in medical research and patient care. The government has signaled that improving diagnostic pathways is a top priority for the coming year. As the technology matures, it could become a standard part of routine gynecological care nationwide. This would mark the end of the “lost decade” that so many women currently endure. The ability to see the disease clearly will also improve the precision of future surgeries. Surgeons will know exactly where to operate before they even enter the modern operating theatre. This reduces the time spent under general anesthesia and improves the overall recovery rates for patients. The future of endometriosis care looks brighter now than it has at any other time. Scientists are hopeful that the full implementation of these scans is only a few years away. Until then, the focus remains on gathering the necessary data to satisfy strict regulatory requirements. The women who participated in this trial have paved the way for a healthier future. Their contribution helps ensure that the next generation will not have to suffer in silence. The English Chronicle will continue to monitor the progress of these vital clinical trials closely. This story serves as a reminder of the power of innovation in modern British medicine. Improving the lives of millions of women remains at the heart of this scientific endeavor. The journey toward a faster diagnosis is finally gaining the momentum it so desperately needs.