Published: 15 May 2026. The English Chronicle Desk. The English Chronicle Online.
A major medical breakthrough has sparked intense debate across the United Kingdom health sector today. A comprehensive new study reveals that prostate cancer screening definitely saves lives. However, researchers quickly warned that the absolute benefit of this testing remains small. Many healthy men could face unnecessary treatments and severe medical complications as a result. This landmark review represents the most detailed analysis of the controversial procedure to date.
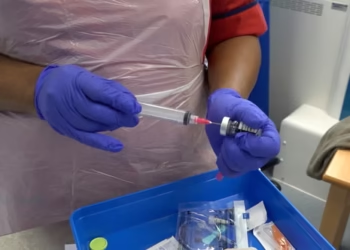
Scientists carefully analysed data from six major clinical trials involving nearly 800,000 international participants. The results showed that prostate-specific antigen testing reduced overall prostate cancer deaths slightly. Specifically, the routine blood screening saved two lives for every 1,000 men tested. This statistic means that 500 men must undergo screening to prevent one single death. The long-term benefit became much more apparent as patients were monitored over several decades.
In particular, the European randomized study of screening for prostate cancer provided crucial data. This specific trial monitored hundreds of thousands of men for 23 years after screening. Professor Philipp Dahm is a leading urologist at the respected University of Minnesota. He also served as the senior author for this important Cochrane review. Dahm confirmed that prostate cancer screening does successfully reduce overall mortality from the disease.
However, he added a strong caveat regarding the timeline required to see results. He noted that patients need a very extended period to realise any actual benefit. Dahm believes this milestone finding will heavily influence healthcare policymakers around the globe. Currently, the United Kingdom does not operate a formal national prostate cancer screening programme. Many other developed nations also avoid universal screening largely because the test remains unreliable.
The standard blood test often fails to differentiate between aggressive and harmless tumours. As well as picking up life-threatening tumours, it detects many completely benign cancers. These minor abnormalities might never cause any health problems during a man’s natural lifetime. Consequently, positive tests often result in men undergoing intense radiotherapy, surgery, or hormone therapy. These invasive medical interventions put patients at high risk of developing permanent complications.
Tragic side effects of these treatments include long-term urinary incontinence and severe impotence. The various studies in the review did not systematically assess overall quality of life. However, the prominent ProtecT trial found significant evidence of post-treatment complications among participants. Between 8% and 47% of men reported major problems with urinary or sexual function. These distressing issues occurred directly after undergoing radiotherapy or surgery for their prostate cancer.
Dr Juan Franco works diligently at the Heinrich Heine University located in Düsseldorf. As the first author of the review, he urged extreme caution regarding interpretation. Franco stressed that the results are not a blanket endorsement of universal screening. He emphasized the very real risks of overdiagnosis and subsequent unnecessary medical treatment. The doctor believes it is vital to have open discussions with individual patients.
He strongly advocates for a healthcare approach known as shared clinical decision making. Prostate cancer remains one of the most common cancers diagnosed in modern men. More than 64,000 cases are diagnosed annually across the United Kingdom alone. Statistics show that one in eight British men will develop the disease. This serious health risk rises significantly to one in four for Black men.
Last year, the UK National Screening Committee advised against widespread prostate cancer screening. They concluded that routine testing was not appropriate for the majority of men. Instead, they recommended a highly targeted programme for specific high-risk genetic populations. This includes men with BRCA1 and BRCA2 mutations linked to aggressive cancers. Government health ministers are currently reviewing this guidance in light of new evidence.
Professor Dahm suggested that screening makes the most sense for specific age brackets. He believes testing is logical when men expect to live another fifteen years. Patients with competing medical comorbidities do not need to worry about prostate cancer. Most forms of this specific disease are incredibly slow-growing and pose little threat. Therefore, older men with other serious illnesses should probably avoid routine blood testing.
The comprehensive review also examined recent technological advances in modern cancer screening methods. These innovative techniques aim to be much more precise than traditional blood tests. They seek to reduce painful, unnecessary biopsies by testing for more specific proteins. Furthermore, doctors are using advanced MRI scans to image the prostate gland clearly. These new imaging methods look highly promising to researchers studying the disease today.
However, the research team stated it was too early to draw definitive conclusions. They cannot yet know if these modern advances will save more lives overall. It also remains unclear if they will successfully cause less harm to patients. David James works as a prominent representative at the charity Prostate Cancer Research. He stated the review clearly demonstrated how screening reduces deaths from the disease.
However, James also noted that diagnosis and treatment have evolved significantly recently. Many of the historical trials used in the review began decades ago. Modern MRI-led diagnostic pathways and highly targeted biopsies are transforming patient outcomes today. Active surveillance techniques and newer biomarker tests are also changing the medical landscape. These innovations alter the delicate balance between the benefits and harms of screening.
Dr Ian Walker serves as an expert leader at Cancer Research UK. He explained why a widespread national screening programme does not currently exist. Walker acknowledged that the test could save up to two lives per thousand. However, he pointed out that thirty additional men would face a diagnosis. Many of these diagnosed men would never have been harmed by the disease.
Instead, they could go on to receive entirely unnecessary and harmful medical treatments. These interventions cause long-term impacts like loss of bladder control and erectile dysfunction. Dr Matthew Hobbs works as an expert director at Prostate Cancer UK. He agreed that the study showed PSA screening could save men’s lives. However, Hobbs quickly added that the current test does not save nearly enough.
He insisted that more research is urgently needed to plug critical evidence gaps. Scientists must find the safest and most effective way to screen British men. This research is essential to ensure that the benefits clearly outweigh the harms. In the meantime, charities must ensure all at-risk men receive accurate information. Men need to make an informed choice about having a PSA blood test.
Every individual must decide what is best for his own health and body. This latest research proves once again that this is not a simple decision. Healthcare professionals must be completely honest with men about the potential clinical benefits. Crucially, they must also outline the potential harms of undergoing the test today.