Published: 1 May 2026. The English Chronicle Desk. The English Chronicle Online
As the UK grapples with a post-pandemic surge in mental health crises, a coalition of medical experts, charities, and bereaved families has launched a renewed “National Urgency” campaign to fix the “catastrophic gaps” in eating disorder care. The push comes as newly released NHS data reveals that hospital admissions for restrictive eating disorders among children under 18 have risen by 12% in the last year alone, despite government promises of a “ring-fenced” mental health budget.
The campaign, spearheaded by the charity Beat, is calling for a mandatory “maximum wait time” of four weeks for adult referrals—aligning them with the standards currently set for children—and an end to the “postcode lottery” of specialist bed availability.
A primary focus of the new campaign is the dismantling of the “BMI-gatekeeping” system, which campaigners argue is a form of “accountability rot” within the healthcare system.
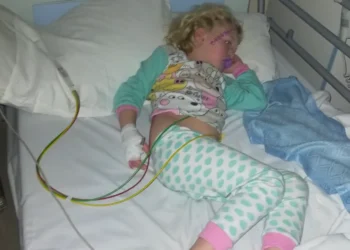
The “Not Sick Enough” Trap: Many patients report being turned away from specialist care because their Body Mass Index (BMI) has not yet dropped to a “life-threatening” level.
The Early Intervention Goal: Experts argue that treating the “mental infrastructure” of the disorder before physical symptoms become acute is both more effective and more cost-efficient.
The Rural Gap: Much like the “weekend gap” in stroke care, access to eating disorder units is heavily skewed toward major cities. In rural areas, patients are often forced to travel over 100 miles for inpatient treatment, severing vital support links with their families.
The push for better care is intrinsically linked to the 2026 digital landscape. While teens are currently trialling life without social media in the “IRL Trial,” the impact of “algorithm-driven” body dissatisfaction remains a key driver of the crisis.
AI-Generated Perfection: The rise of hyper-realistic AI “influencers” has created a new, unattainable standard of beauty. Campaigners are calling for “clear labelling” on AI-generated human images to prevent further damage to adolescent self-esteem.
The “Fit-Check” Culture: Even as the “anti-fraud” digital task force targets financial scammers, health advocates argue that “pro-anorexia” communities are successfully bypassing platform filters by using “coded” language and “shadow” accounts.
The “Boredom” Vulnerability: Preliminary results from the social media hiatus trials suggest that while some teens feel “liberated,” others experience a “dopamine desert” that can lead to a fixation on food and exercise as a primary source of control.
The campaign features a moving testimony from families who have lost loved ones to the illness. They argue that the “slow-motion” nature of the disease often leads to a lack of urgency in the primary care sector.
“If my daughter had a physical tumor, she would have been operated on in weeks,” said one mother. “But because her illness was ‘in her head,’ we were told to wait. In this country, justice—and care—should not have an expiry date based on the type of illness you have.”
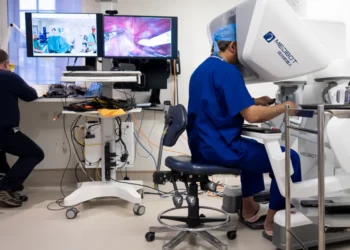
The government’s response, expected during the King’s Speech on May 13, is rumored to include a “pioneer” pilot scheme for “autonomous monitoring”—using wearable tech similar to the smart-suture robots to track vital signs in high-risk patients remotely.
The eating disorder crisis is being viewed as a symptom of a broader “national security emergency” of societal well-being.
The Financial Link: With “billions of meals at risk” due to the fertilizer crisis and fuel prices hitting 157p, the “anxiety of scarcity” is being cited as a potential trigger for those with a predisposition to disordered eating.
The “Golden Tone” of Recovery: Charities are highlighting “success stories” of those who have navigated the system, emphasizing that with the right investment, recovery is not just possible—it is probable.
As the Southbank Centre celebrates 75 years of British culture and RHS Wisley’s wisteria blooms, the message from the “Improved Action” campaign is one of hope balanced with a demand for radical change. “We are tired of ‘awareness weeks’,” said a Beat spokesperson. “We need beds, we need clinicians, and we need to stop weighing people to decide if they deserve to live.”