Published: 27 April 2026. The English Chronicle Desk. The English Chronicle Online.
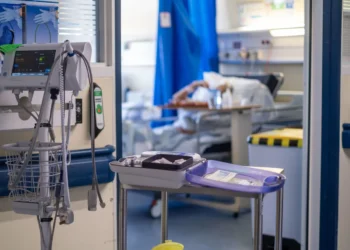
The landscape of mental health care in the United Kingdom is facing a truly alarming situation. A recent and comprehensive poll reveals that four-fifths of mental health nurses find their workloads unmanageable. This staggering statistic highlights a deep systemic failure that is currently impacting thousands of vulnerable patients across the nation. Specialist nurses are working tirelessly but are finding it nearly impossible to keep up with the overwhelming demands. High caseloads coupled with severe understaffing have created a dangerous environment for both staff and those seeking essential care. The professional voices of those on the frontline now echo a singular and desperate plea for urgent government action.
Professor Nicola Ranger, the general secretary of the Royal College of Nursing, recently described this situation as a perfect storm. She explained that nurses are trapped in a cycle where rising demand consistently outpaces the capacity of the current workforce. Consequently, patients are the ones paying the ultimate price by missing out on crucial and often life-saving support services. The data indicates that only one-fifth of specialist nurses feel their current workload is manageable, which is a devastating figure for the sector. This imbalance places an immense psychological burden on staff who enter the profession to provide compassionate care to those in need.
The findings from the Royal College of Nursing survey paint a bleak picture of daily operations within the mental health sector. Half of the specialist nurses who responded to the survey stated that their patients frequently come to harm due to these extreme caseloads. Furthermore, a full quarter of respondents reported that time pressures lead to daily issues concerning patient deterioration, relapse, or even self-harm. These are not merely administrative failures but are significant incidents that affect the lives of real people who are already struggling with their mental health. Nurses expressed profound distress as they watch their patients suffer while they remain unable to provide the necessary support.
Nearly two-thirds of the nurses surveyed noted that their specific caseloads have increased significantly over the past three years. Many pointed toward excessive administrative burdens and a restrictive tick-box culture as the primary culprits behind this decline in care quality. These bureaucratic demands siphon away precious hours that should be dedicated entirely to direct patient engagement and therapeutic support. The survey further suggests that the total demand for services has grown more than twice as fast as the actual number of nurses available to meet that demand. This widening gap between need and provision is causing a collapse in the standard of care expected within the National Health Service.
The human element of this crisis is best illustrated by the testimony of those working on the ground level. One nurse shared that vulnerable patients seeking help from her trust often wait weeks for even a basic response. In some truly concerning instances, these patients might not be contacted by the service at all despite their clear and urgent needs. Another nurse captured the severity of the situation by remarking that the environment feels incredibly dangerous. She even admitted that she frequently awaits the day she might be called to explain these systemic failures in a coroner’s court. Such statements reflect a profound sense of helplessness and fear among highly dedicated and trained professionals.
Statistical data confirms the massive scale of this challenge, particularly regarding community mental health services in England. Between October 2022 and 2025, the number of individuals accessing these services rose by 38 percent. Specifically, this means the figures climbed from roughly 499,000 patients to nearly 690,000 in just three short years. Conversely, the nursing workforce only grew by 15 percent, moving from approximately 20,000 to just over 23,000 staff members. With such a massive discrepancy, it is perhaps unsurprising that only 12 percent of nurses feel they have enough time to care for their patients properly.
These warnings align perfectly with previous concerns raised by the Care Quality Commission earlier this year. Their report indicated that one-third of people seeking mental health support must wait at least three months for an appointment. Furthermore, the report revealed that half of the individuals contacting crisis services for children and young people failed to receive the immediate help they required. These figures suggest that the crisis is not limited to one specific area but is a broad issue affecting various demographics and age groups. The cumulative effect of these delays is a deteriorating mental health landscape that requires a bold and immediate national response.
Professor Ranger argues that growing this crucial workforce must become a primary priority for the UK government. She advocates for sustained and significant investment in community mental health nursing to stabilize the current situation. Additionally, the Royal College of Nursing believes that a massive investment in digital infrastructure would alleviate many of the administrative burdens currently plaguing these teams. Modernizing the way data is handled could return valuable hours to the nurses who desperately need to spend time with their patients. Without these structural changes, the current model of care remains unsustainable and prone to further decline.
Charitable organizations like Mind are also speaking out about the immense pressures currently placed upon frontline mental health workers. Tom Pollard from the charity noted that staff are clearly trying their best to deliver high-quality care despite the overwhelming obstacles. However, the combination of growing demand and administrative burdens makes this an increasingly impossible struggle for even the most dedicated employees. He emphasized that people need timely and high-quality care delivered by professionals who are not stretched beyond their reasonable limits. Without such support, the safety of patients remains at significant risk, and their chances of successful recovery diminish significantly.
The government maintains that it is taking the necessary steps to address these complex and long-standing problems. A spokesperson for the Department of Health and Social Care stated that community mental health nurse numbers have increased by 26 percent since July 2024. They acknowledged that there is still much more work to do to reach an ideal standard of service provision. As part of this commitment, they are investing a record 16.1 billion pounds into mental health services this year. These funds are intended to support the reform of the Mental Health Act and the hiring of thousands more mental health workers nationwide.
Furthermore, the government intends to upgrade existing mental health infrastructure to ensure it is fit for the future. Whether these measures will be enough to resolve the deep-seated issues identified by the nursing staff remains a topic of intense national debate. Nurses and patients alike are calling for visible and immediate improvements that go beyond simple promises of future funding. The reality of today is that the system is buckling under the weight of excessive expectations and limited resources. Ensuring that the most vulnerable members of society receive the care they deserve must remain the central focus of these ongoing reforms. As the country moves forward, the success of these initiatives will be measured by the ability of nurses to provide effective and timely support to every patient who reaches out for help.