Published: 01 January 2026. The English Chronicle Desk. The English Chronicle Online.
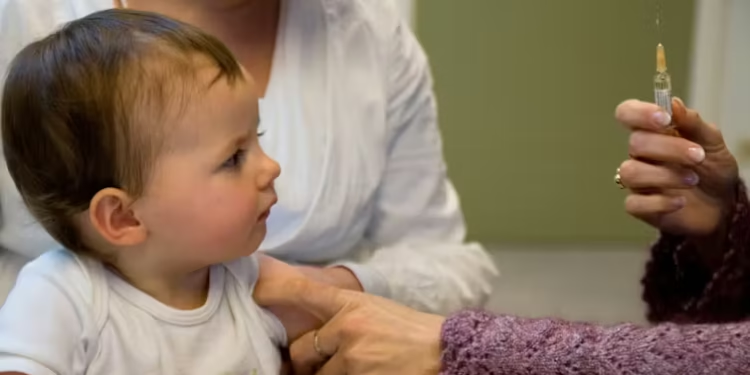
England is preparing a significant shift in public health delivery as home vaccines are set to reach children directly where they live. The move follows mounting concern that thousands of children are starting school without essential protection. Health officials believe offering home vaccines could restore confidence, remove access barriers, and rebuild trust with families struggling to engage traditional services. The initiative marks one of the most proactive immunisation strategies seen in recent years, responding to declining uptake across nearly every childhood programme.
Under a new NHS-backed pilot, specially trained health visitors will begin delivering routine childhood vaccinations inside family homes. The £2 million scheme launches this month across twelve pilot areas in England. These include parts of London, the Midlands, the North East, Yorkshire, the North West, and the South West. Officials hope home vaccines will close dangerous gaps that leave children exposed to preventable diseases.
Health visitors, often nurses or midwives with specialist training, already support families with children under five. Their role focuses on early intervention, child development, and safeguarding wellbeing. By enabling them to administer vaccines, the NHS aims to reach families facing complex challenges. These include missed GP registrations, financial pressure, language difficulties, transport barriers, and childcare constraints. For many households, home vaccines may be the first practical opportunity to complete routine immunisations.
The decision follows alarming data reviewed by public health authorities. The World Health Organization advises that at least ninety-five percent vaccine coverage is required to maintain herd immunity. In England, no major childhood vaccine met that target during 2024 and 2025. Regional inequalities widened, with some urban communities falling far below safe thresholds. Health leaders warn these gaps create conditions for outbreaks, hospital pressure, and avoidable tragedy.
NHS systems will identify eligible children using GP records, health visitor notes, and local authority databases. Families will be contacted directly and offered appointments at home. Health visitors will receive additional training to administer vaccines safely and address parental concerns. Conversations around hesitancy, misinformation, and fear will be central to the approach. Officials stress that home vaccines are voluntary, designed to support, not pressure, families.
Wes Streeting, the Health Secretary, described the policy as a practical response to inequality. He said many parents want to protect their children but face daily pressures that derail appointments. By bringing services to the doorstep, he argued, the NHS is meeting families where they are. Streeting emphasised that rebuilding vaccination rates is essential to fixing a strained health system and preventing long-term harm.
The initiative arrives during a difficult winter for the NHS. Hospitals remain under extraordinary pressure from flu, respiratory illnesses, and seasonal viruses. While flu vaccination rates improved this year, officials say uptake remains uneven. Health leaders continue urging unvaccinated people to come forward, warning that winter pressures could intensify rapidly as temperatures drop further.
Concerns around childhood vaccination extend beyond seasonal illness. Data from the UK Health Security Agency show that uptake of the measles, mumps, and rubella vaccine has fallen to historic lows. Just over ninety-one percent of five-year-olds received one MMR dose in 2024 and 2025. Fewer than eighty-four percent completed both doses, leaving large numbers vulnerable. These figures represent the lowest levels recorded in over a decade.
The consequences are no longer theoretical. In July, a child in Liverpool died after contracting measles, the first such death in the United Kingdom in ten years. Only seventy-three percent of children in the city have received both recommended MMR doses. Public health experts say outbreaks could become more frequent unless coverage improves quickly. They believe home vaccines could prevent similar tragedies by reaching families earlier.
International comparisons deepen concern. According to the World Health Organization, the United Kingdom now ranks lowest among G7 nations for MMR uptake. Globally, vaccine coverage has stalled or reversed in many countries since the pandemic. Disruption to health services, misinformation online, and declining trust have combined to erode progress built over decades. England’s decision to trial home vaccines reflects a broader effort to adapt systems to new realities.
Other routine immunisations show similar declines. Coverage for the Hib and MenC vaccine, protecting against meningitis and serious bacterial infections, dropped below eighty-nine percent among five-year-olds. Uptake of the preschool booster covering polio, tetanus, diphtheria, and whooping cough fell to just over eighty-one percent. This leaves nearly one in five children unprotected when starting primary school, a figure health leaders describe as unacceptable.
Alongside the home vaccination scheme, the NHS is expanding the childhood programme with the rollout of a chickenpox vaccine. From this week, the jab will be available free through GP practices across England. Previously, families often paid privately, with costs reaching one hundred and fifty pounds. The vaccine will be delivered as part of a combined MMRV immunisation, offering protection against measles, mumps, rubella, and varicella.
Ministers believe the chickenpox vaccine will reduce serious complications and ease pressure on parents and employers. Chickenpox remains highly contagious, often forcing parents to take time off work. Health officials expect the new programme to protect around five hundred thousand children each year. Over time, the combined MMRV is expected to replace the existing MMR schedule.
Public reaction to home vaccines has been mixed but largely supportive. Many parents welcome the convenience and reassurance of seeing trusted professionals at home. Others have raised questions about capacity, cost, and workforce strain. Nursing unions say success depends on sufficient staffing and clear safeguards. The Department of Health insists the pilot is carefully resourced and will be independently evaluated.
If the trial proves effective, the government plans a nationwide rollout by 2027. Health leaders view the programme as a test case for more flexible, community-based care. They argue that restoring vaccine confidence requires visibility, consistency, and relationships built over time. In that context, home vaccines represent more than logistics; they signal a shift in how the NHS engages families.
As England faces rising disease risks and widening health gaps, officials stress urgency. Preventable illnesses remain a serious threat when coverage slips. By delivering vaccines directly to front doors, the NHS hopes to rebuild protection, trust, and resilience. For thousands of children, home vaccines could mean a safer start to school and a healthier future.