Published: 18th August 2025. The English Chronicle Desk
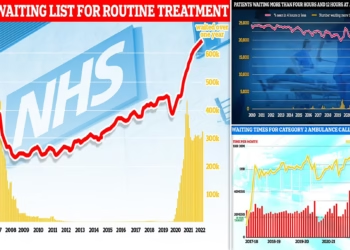
Pressure on NHS cancer services in England has continued to mount, as the latest data reveal mixed progress in meeting critical targets for diagnosing and treating cancer. These waiting times not only reflect the efficiency of the health system but also have profound implications for patients’ outcomes, stress levels, and overall wellbeing. Early diagnosis and prompt treatment are vital in improving survival rates, as cancers detected at an early stage are more amenable to successful treatment and are less likely to have spread.
Recent figures for June 2025 show that the NHS met the Faster Diagnosis Standard, with 76.8 percent of patients receiving a diagnosis—or having cancer ruled out—within 28 days of an urgent referral, exceeding the 75 percent target. This represents a positive development, providing some reassurance to patients that initial investigations are being carried out without excessive delays
However, significant challenges remain in other key measures. The 62-day referral-to-treatment standard, which requires patients to begin treatment within two months of an urgent referral, was missed once again, with only 67.1 percent of patients receiving timely care compared to the 85 percent target. This shortfall has been persistent, with the target not met since December 2015. Similarly, the 31-day decision-to-treat standard, which measures the time from treatment planning to treatment initiation, fell short at 91.7 percent, below the 96 percent benchmark. These delays are of particular concern because research indicates that even a four-week postponement in surgery can increase the risk of mortality by six to eight percent for certain cancers.
The impact of these delays is not uniform across all cancer types. Some aggressive cancers are prioritised, allowing patients to receive faster intervention where possible, while others may face extended waits due to treatment planning complexities or the need for prehabilitation to maximize recovery prospects. Nonetheless, the increasing frequency of missed targets highlights a systemic challenge: patients in need of potentially lifesaving treatments are enduring longer periods of anxiety and uncertainty.
While delays are troubling, medical professionals emphasize that patients should not hesitate to seek care if they experience concerning symptoms. Timely referral remains critical, and physicians generally escalate urgent cases to minimize risk.
The broader context shows that progress in cancer survival in the UK has slowed in recent years. Despite remarkable advances over the past five decades, the country lags behind comparable international healthcare systems. With nearly one in two people expected to face a cancer diagnosis during their lifetime, the pressures on early detection, timely treatment, and risk factor management are increasingly acute.
Government initiatives, such as the recently published Ten-Year Health Plan, outline ambitions to shift from analogue to digital, from reactive treatment to prevention, and from hospital-centric care to community-focused approaches. While the plan reiterates commitments to reducing waiting lists and improving NHS productivity, it does not specifically address cancer waiting times, leaving a gap in strategic focus for one of the most pressing public health challenges.
The National Cancer Plan is expected to provide more targeted measures, including investment in earlier diagnosis, sustainable delivery of best practice treatments, reduction of major risk factors, and expansion of research-driven healthcare. Success will depend on clearly defined governance structures, accountability mechanisms, and sufficient resourcing to ensure that ambitious targets translate into tangible improvements for patients.
As the NHS continues to grapple with long waiting lists and systemic pressures, the call for urgent, coordinated action grows stronger. Both current and future cancer patients depend on timely reforms to ensure that delays do not compromise survival outcomes or exacerbate anxiety during already stressful periods. Experts and patient advocacy groups are urging the Secretary of State for Health and Social Care to prioritize the National Cancer Plan’s implementation, ensuring that improvements in diagnosis, treatment, and patient support become a reality rather than a policy aspiration.
These figures underscore a critical tension within the NHS: while some progress is evident in early diagnostic targets, significant gaps remain in delivering treatment on schedule. The challenge now lies in sustaining the gains achieved, addressing the persistent shortfalls, and protecting patients from the potentially devastating consequences of delayed care.