Published: 12 August — The English Chronicle Desk
Violence against nurses working in Accident and Emergency (A&E) departments across England has surged dramatically over the past six years, according to newly released NHS figures. The data reveals a 91% increase in violent incidents against nursing staff, rising from 2,122 cases in 2019 to 4,054 in 2024. Much of this increase has been linked to patients’ frustration over long waiting times and systemic pressures within emergency care settings.
Nurses have been subjected to a range of assaults, including being punched, spat at, and even threatened with acid attacks. Some have faced the terrifying experience of having guns pointed at them. These distressing realities were highlighted by the Royal College of Nursing (RCN), which secured the figures through freedom of information requests to NHS trusts across England.
Professor Nicola Ranger, General Secretary of the RCN, described the situation as “an ugly truth behind shocking figures,” emphasising that the rising violence is a symptom of broader systemic failures in the NHS. She underlined that every single incident is unacceptable and that frontline staff are being put under immense strain through no fault of their own.
Accounts from frontline nurses paint a grim picture of working conditions. Rachelle McCarthy, a charge nurse in the East Midlands, recalled being punched in the face by an agitated patient. Senior sister Sarah Tappy from east London recounted a harrowing incident in which a patient knocked her unconscious with a punch to the head. Across the south-west of England, nurses have reported being pinned against walls and suffering assaults to sensitive areas of the body.
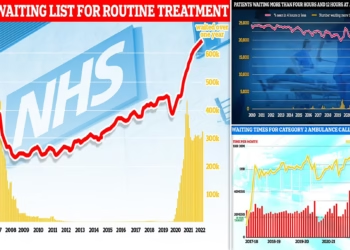
The rising violence is mirrored by the increasing number of long waits patients face in A&E departments. Hospitals such as Southmead in Bristol saw attacks on staff rise from 83 in 2019 to 152 last year. Manchester Royal Infirmary’s incidents doubled from 39 to 79, while Maidstone hospital in Kent experienced a sharp rise from 13 to 89 attacks.
Daniel Elkeles, CEO of NHS Providers, expressed deep concern about the findings. He stressed the vital importance of ensuring NHS staff have safe and respectful workplaces free from threats and intimidation. Elkeles acknowledged that long delays in treatment contribute to patient frustration but reassured that efforts to reduce waiting times are ongoing.
The RCN has called for urgent government intervention to address the growing violence, linking it closely to the broader challenges of overcrowded hospitals, widespread “corridor care,” and persistent nursing shortages. A separate analysis by the union also revealed a staggering increase in the number of patients waiting over 12 hours in A&E, a figure that has multiplied twentyfold since 2019.
To combat the rising threat, many hospitals have bolstered security by increasing personnel, providing stab-proof vests to clinical staff, and installing additional CCTV coverage. However, Rebecca Smith, director of system and social partnership at the NHS Confederation, warned that the near doubling of attacks is “deeply worrying” and underlined that violence at work severely impacts staff wellbeing, retention, and the quality of patient care.
The figures reflect only reported incidents at the largest A&E units of NHS trusts, suggesting the true scale of violence may be even higher. The most recent NHS staff survey revealed that one in seven workers experienced physical violence in the past year, highlighting the widespread nature of the issue.
Duncan Burton, Chief Nursing Officer for England, condemned the violence as “totally unacceptable” and urged NHS staff to report all incidents to enable appropriate legal action. Health Secretary Wes Streeting expressed his outrage, affirming that nurses deserve to work free from intimidation and violence and pledging that perpetrators would face the full force of the law.
As pressures mount on emergency services, the harrowing accounts of assaulted nurses bring urgent attention to the need for systemic reforms to protect the NHS workforce and improve patient care environments across the country.