Published: 22 October 2025. The English Chronicle Desk. The English Chronicle Online.
For the first time, researchers have ranked the physical side effects of different antidepressants, revealing significant differences between medications that could influence patient health and adherence. The study, conducted by academics from King’s College London and the University of Oxford, examined 151 studies covering 30 commonly prescribed drugs and over 58,500 patients, focusing on the initial eight weeks of treatment.
Findings showed that some antidepressants can cause patients to gain up to 2 kilograms in weight or experience fluctuations in heart rate of as much as 21 beats per minute. With approximately eight million people in the UK taking these medications, experts warn that selecting the right drug for each individual could have a substantial impact on overall health outcomes.
Professor Oliver Howes highlighted the importance of considering these differences not just for individual patients, but across the population, as even modest effects could translate to significant public health consequences. Dr Atheeshaan Arumuham emphasised that no two antidepressants are the same, and their effects can be clinically meaningful, including an increased risk of heart attack or stroke in some cases.
The study’s ranking aims to guide doctors and patients in making better-informed decisions. Dr Toby Pillinger urged individuals not to discontinue their medication abruptly but encouraged engaging in shared decision-making with healthcare professionals to find the most suitable treatment.
Using hypothetical patient examples, researchers illustrated how preferences and existing health conditions could influence drug choice. For instance, a patient prioritising avoiding weight gain might be recommended a different antidepressant than someone with high blood pressure or elevated cholesterol.
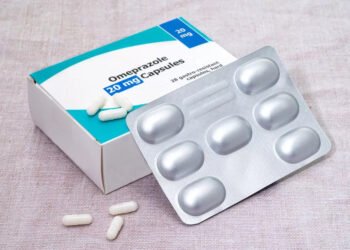
While some drugs, like amitriptyline, may cause weight gain, heart rate changes, and blood pressure increases, they can also provide benefits such as improved sleep and pain management. The study found that SSRIs (selective serotonin reuptake inhibitors) – including paroxetine, citalopram, escitalopram, and sertraline – generally produced fewer physical side effects. Fluoxetine (Prozac), another SSRI, was linked to weight loss but increased blood pressure.
Professor Andrea Cipriani from the University of Oxford stressed that the findings do not mean current prescriptions are inappropriate, but suggested that the dominance of three SSRIs (citalopram, sertraline, and fluoxetine) covering 85% of UK prescriptions limits patient choice. A more personalised approach could ensure better treatment outcomes.
Researchers are developing a free online tool to help doctors and patients select the most appropriate antidepressant, although changing prescribing culture within the NHS remains a challenge. The study only examined the first eight weeks of treatment, but early evidence suggests that observed changes in physical health may persist over time. Dr Prasad Nishtala from the University of Bath, not involved in the research, noted that long-term cumulative risks could be higher, particularly in patients with chronic depression.
The study represents a crucial step towards more personalised mental health care, highlighting the importance of considering physical side effects alongside therapeutic benefits when prescribing antidepressants.