Published: 10 December 2025. The English Chronicle Desk. The English Chronicle Online.
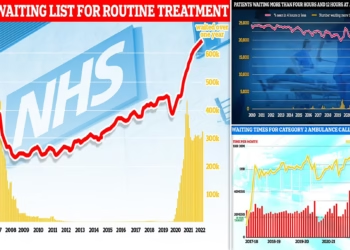
Corridor care has become a widespread and urgent problem across UK hospitals, doctors have warned, as a new study reveals alarming statistics on the practice. One in five patients admitted to emergency departments is reportedly treated in hallways, offices, cupboards, or other unsuitable areas, exposing them to unsafe and undignified conditions. Researchers say the phenomenon is routine, despite national guidance explicitly stating that such care is unacceptable.
The study, conducted by the Royal College of Emergency Medicine’s (RCEM) trainee emergency research network (Tern), surveyed 165 emergency departments in March 2025, capturing five separate data snapshots. Analysis found that 17.7% of patients were receiving treatment in “escalation areas,” spaces not intended for routine patient care unless department capacity is exceeded. These areas include corridors, waiting rooms, doubled-up cubicles, offices, cupboards, and ambulances delayed outside.
Researchers publishing in the Emergency Medicine journal emphasised that corridor care constitutes a “significant patient safety issue.” They noted that while the temporary use of such spaces may be necessary during extreme pressure, the findings illustrate systemic normalisation of this practice. Dr Ian Higginson, RCEM president, described the findings as evidence that corridor care is “endemic” across UK emergency departments.
“The stark reality mirrors the experiences reported by our members nationwide,” Dr Higginson said, highlighting rising volumes of patients awaiting care. He cited instances of patients enduring waits as long as two days for hospital beds. Vulnerable populations—including elderly people, children, and those with mental health conditions—are disproportionately affected, he added.
The research comes amid mounting concerns over long-term patient neglect. In October, The Guardian reported that nearly 150,000 people aged 90 or over in England are forced to wait more than 12 hours in emergency departments each year. Some patients endured several days in corridors, often without access to basic care, including pain relief or sanitary conditions, and in proximity to other critically ill patients.
Dr Higginson stressed that the study’s March data likely underrepresents the problem, as corridor care typically intensifies during winter. He warned that prolonged waits in emergency departments have tangible consequences for patient survival, estimating that one excess death occurs for every 72 patients who wait between eight and twelve hours before admission.
Despite widespread awareness of the crisis, Dr Higginson criticised successive governments for failing to prioritise patient safety adequately. “It cannot be dismissed as mere seasonal strain or flu outbreaks,” he said. “We fear severe gridlock in hospitals this winter if decisive action is not taken.”
Last week, Health Secretary Wes Streeting pledged to eliminate corridor care in hospitals by the next general election, stating the government’s commitment to improving patient dignity and safety. The Department of Health and Social Care reaffirmed that corridor care is “unacceptable” and that publication of corridor waiting figures will begin immediately, enabling transparency and accountability. A spokesperson highlighted that while addressing the crisis will take time, some “green shoots of recovery” are already visible.
The research underlines the need for urgent reform within the NHS, emphasising that systemic overcrowding and delays in emergency care continue to jeopardise patient wellbeing. Experts argue that addressing the root causes of corridor care—ranging from chronic underfunding to staffing shortages—must remain a priority to ensure the safety and dignity of all patients.
Patients, healthcare professionals, and advocacy groups have called for comprehensive strategies to prevent the continued normalisation of corridor care, urging policymakers to enforce stringent standards and provide sufficient hospital capacity. The RCEM research reinforces that corridor care is no longer an occasional emergency measure but a persistent feature of UK healthcare, requiring immediate attention to prevent further harm.
While health authorities point to initial improvements, doctors insist that without systemic interventions, vulnerable populations will continue to experience undignified treatment in hospitals nationwide. The findings serve as a sobering reminder that healthcare systems must adapt proactively to meet patient needs, ensuring safe and timely care throughout the year.