Published: 30 December 2025. The English Chronicle Desk. The English Chronicle Online.
Emergency departments across the United Kingdom are facing an escalating crisis, as corridor care becomes an accepted reality rather than an emergency measure. Senior clinicians are warning that what was once viewed as unacceptable has now been normalised, placing patients at serious risk and pushing exhausted staff to breaking point. The comments come amid mounting evidence that long waits for hospital beds are contributing to thousands of avoidable deaths each year.
Dr Ian Higginson, president of the Royal College of Emergency Medicine, has described the situation as “big trouble” for the NHS, arguing that public outrage has failed to match the scale of harm being caused. He has warned that only a small number of hospitals have managed to avoid placing patients on trolleys in corridors, while the majority struggle daily with overcrowded emergency departments.
Corridor care, once considered a last resort during extreme pressure, has become so common that patients often expect it. According to Dr Higginson, many people arriving at A&E are no longer surprised to find themselves treated in hallways, storage spaces, or other unsuitable areas. This acceptance, he says, masks a profound failure of the healthcare system and undermines the quality and safety of care being delivered.
Medical staff working in these conditions report that providing effective treatment in corridors is nearly impossible. Privacy is compromised, infection risks increase, and critical monitoring becomes more difficult. Doctors and nurses are forced to make rapid decisions in crowded, noisy environments, often without access to essential equipment. Dr Higginson has stressed that clinicians simply cannot deliver safe and dignified care under such circumstances.
Earlier this year, the Royal College of Emergency Medicine released estimates suggesting that more than 16,600 patient deaths were linked to excessively long waits in A&E for hospital beds during the previous year. This equates to around 320 deaths every week, a figure that has shocked many within the profession but has yet to provoke decisive action at the highest political level.
Dr Higginson has drawn stark comparisons to other public safety disasters. He argued that if similar numbers of people were dying annually in transport accidents, there would be immediate national outrage and urgent reform. The lack of comparable reaction to A&E-related deaths, he believes, reflects a dangerous desensitisation to suffering within the health system.
Further analysis published earlier this month revealed that nearly one in five patients treated in UK emergency departments during March were cared for in so-called escalation areas. These areas include corridors and other non-clinical spaces not designed for patient treatment. Dr Higginson suspects that the situation has since worsened, mirroring broader signs of deterioration across the NHS.
The findings highlight how winter pressures, staff shortages, and delayed discharges combine to overwhelm hospitals. As beds remain occupied by patients who cannot be safely discharged, emergency departments become bottlenecks, forcing new arrivals to wait hours or even days for admission.
In December, Health Secretary Wes Streeting pledged to end corridor care in hospitals in England by the next general election, if not sooner. While the commitment has been welcomed, frontline clinicians remain cautious, noting that similar promises have been made before without lasting change. They argue that eliminating corridor care will require sustained investment and systemic reform rather than short-term fixes.
Dr Higginson has criticised what he sees as an overemphasis on quick, inexpensive solutions. Efforts to redirect patients away from hospitals, he said, may help at the margins but do not address the underlying causes of overcrowding. He insists that the crisis is solvable, but only with sufficient political will and a willingness to confront uncomfortable truths.
At the heart of the problem, he argues, is hospital inefficiency driven by chronic underfunding and workforce shortages. Increasing staffed bed capacity, improving patient flow, and strengthening community and social care services are essential steps. Without these changes, patients who are medically fit to leave hospital remain stuck, preventing others from being admitted from A&E.
The human cost of the crisis extends beyond patients to the staff caring for them. Many emergency clinicians describe being “run ragged,” working long shifts under relentless pressure. Burnout, moral injury, exhaustion, and symptoms consistent with post-traumatic stress disorder are increasingly reported among healthcare workers. Dr Higginson has warned that failing to improve conditions risks driving experienced staff out of the profession altogether.
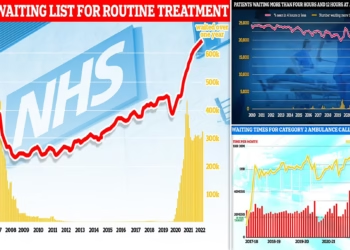
Official NHS figures underscore the scale of the challenge. In November alone, more than 50,000 people in England waited over 12 hours in A&E from the decision to admit them to the point of being given a hospital bed. For many, these waits occurred in corridors, where basic comfort and dignity are difficult to maintain.
NHS England has acknowledged that such delays are unacceptable. A spokesperson said the organisation is working to free up beds by accelerating discharges for patients who are medically fit and expanding access to community-based care. This winter, productivity specialists and regional experts have been deployed to support hospitals in reducing corridor care and improving patient experience.
The Department of Health and Social Care has also conceded that corridor care is undignified and unacceptable. A spokesperson said the government inherited a difficult situation but remains determined to bring the practice to an end. Officials point to signs of recovery, including improvements in four-hour A&E performance and faster ambulance response times for life-threatening conditions.
However, critics argue that these improvements are fragile and unevenly distributed. They warn that focusing on headline targets risks obscuring the lived reality of patients waiting in unsuitable spaces. For those experiencing pain, fear, or confusion in crowded corridors, assurances of future reform offer little immediate comfort.
As winter continues to place intense strain on the NHS, the debate over corridor care has become a symbol of wider systemic failure. Clinicians like Dr Higginson insist that accepting the practice as normal is not only dangerous but morally wrong. They argue that public awareness and political urgency must match the severity of the harm being caused.
The coming months will test whether pledges to end corridor care translate into meaningful change. For now, emergency departments remain on the frontline of a crisis that many believe has been allowed to deepen for too long. The question facing policymakers is whether they are prepared to act decisively before normalisation turns into tragedy.